A study published in 2012 found that more than 64 million Americans aged 30 or older had periodontal (gum) disease. Gum disease, also known as periodontitis, is a severe infection of the gums caused by an immune response to imbalanced oral bacteria. Inflammation from periodontal disease can damage gums, destroy the jawbone, and lead to tooth loss. Several studies have shown an association between periodontal disease and other systemic diseases such as heart disease, diabetes, cancer, and dementia. But what about the association between dental health and kidney disease? In this blog, I am going to explore that link.

Periodontal disease and systemic inflammation
The oral microbiome produces metabolic by-products in the mouth. Some of these by-products leak into the blood stream and lead to a low-grade systemic inflammation. Studies have shown that patients with severe periodontitis have elevated levels of pro-inflammatory mediators and increased neutrophil numbers in the blood. In fact, successful treatment of gum disease was associated with improvement in inflammatory markers. Many of these inflammatory markers have been linked to heart disease, diabetes, and other diseases. This may explain the link between periodontal disease and systemic diseases.
Join us in the fight against kidney disease and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
CKD is an inflammatory state
Low-grade inflammation has been shown to be an integral aspect of chronic kidney disease (CKD). Here, too, inflammatory markers were found to be elevated. As kidney function worsens, the levels of these markers increase in the body. They also increase with increasing urine protein (albuminuria), which is common in CKD.
On the other hand, an evaluation of the Chronic Renal Insufficiency Cohort (CRIC) study found that elevated inflammatory markers were associated with rapid progression of kidney disease. So, the relationship between inflammation and kidney disease is bidirectional. CKD can lead to inflammation and inflammation can lead to and worsen CKD.
Download Your Copy!
Can gum disease cause kidney problems?
Periodontitis can increase the risk of CKD by direct and indirect effects. Directly, periodontitis increases systemic inflammatory burden leading to an increased incidence of CKD. In a recent review of 37 studies, researchers found strong evidence that periodontitis is associated with an increased risk for CKD. This association remained strong after adjusting for other risk factors.
Periodontitis can also increase the risk for CKD indirectly by increasing the risk for insulin resistance and diabetes. In this study, diabetes increased the odds of CKD by twofold, and 6.5% of this effect was mediated by periodontitis.
In addition, some of the increased risk of CKD may have to do with genetics. For example, variants in vitamin D receptor gene were associated with CKD during inflammatory conditions caused by periodontal disease.
There is not a lot of data on how treating gum disease affects CKD. However, in this pilot study, researchers found that treating severe chronic periodontitis for 180 days led to improvement of all periodontal clinical parameters. This was associated with statistically significant improvement in kidney function and markers of inflammation.
CKD and periodontitis: Does kidney disease affect oral health?
On the other hand, CKD can affect oral health by inducing gum overgrowth (known as gingival hyperplasia), dry mouth, calcification of root canals, and delayed eruption of teeth in children. These can lead to increased risk of periodontal disease. In addition, severe periodontal disease was found to be more common in patients with more severe CKD.
Kidney disease, gum disease, and nutrition
There is a triangular interaction between nutrients, CKD, and periodontal disease. Protein wasting that is common in kidney disease, for example, can increase the risk of periodontal disease. Omega-3 fatty acids, on the other hand, were found to be beneficial in the management of chronic periodontitis. Many other nutrients and micronutrients that can be altered in CKD were also associated with periodontal disease.
CKD medications may cause gum and teeth problems
Some of the medications that are used for patients with CKD can also increase the risk for periodontitis. Medications such as calcium channel blockers that are used to treat blood pressure can lead to gum swelling and overgrowth. This was also noted in some transplant medications such as cyclosporine. Other medications can be associated with dry mouth, which can promote gum and teeth problems. These include ACE inhibitors, calcium channel blockers, betablockers, and diuretics.
The bottom line on chronic kidney disease and oral health
Both periodontal disease and CKD are associated with low-level systemic inflammation. The association between the two is bidirectional. Periodontal disease can increase the risk for CKD and the rate of its progression. On the other hand, CKD can also worsen periodontal disease. Paying attention to oral health is essential for the prevention of many chronic diseases. It is also crucial for preventing or slowing down the progression of CKD.
The post Can Gum Disease Cause Kidney Problems? appeared first on Integrative Kidney.]]>
Cold exposure
Cold exposure, such as cold showers, has many benefits for kidney patients. It increases endorphins and fights off depression. It improves metabolism and circulation. Most importantly, it stimulates the vagus nerve and improves renal circulation. It may also soothe itchy skin which is common in CKD patients. In addition, cold showers help with post-workout muscle soreness.
The benefits of a cold shower begin when the water temperature dips to 60 degrees Fahrenheit. This is 40 degrees lower than the typical steamy shower. To take a cold shower, start with your usual hot shower, then turn the knob to cold at the end of your shower. Lower the temperature gradually at the end of your shower every day. The benefits start with thirty seconds under the cold water. Maximum benefits are reached in three minutes.
Join us in the fight against kidney disease and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
Vagus nerve breathing exercises
Deep and slow breathing can activate the parasympathetic system. In fact, deep breathing is one of the best ways to lower stress in the body. It sends messages to the brain to calm down and relax by activating the vagus nerve which helps lower heart rate and blood pressure. There are various ways to perform deep breathing. Here, I will discuss the 4-7-8 breathing technique.
This technique uses belly breathing. It can be performed sitting or lying down as follows:
- Start by putting one hand on the belly and the other one on the chest.
- Take a deep slow breath from the belly while silently counting to 4. The chest should not move.
- Hold the breath while silently counting to 7.
- Breathe out completely while silently counting to 8.
- The process can be repeated 5 to 10 times until feeling relaxed.
Singing, humming, chanting, and gargling
These activities have also been shown to improve heart rate variability and can also activate the vagus nerve because it is connected to the vocal cords. These benefits can be achieved by 10 minutes of singing, humming, chanting, or gargling every day.
Probiotics
The fact that probiotics have been found to support stimulation of the vagus nerve is another piece of evidence for the importance of the gut-brain axis. Healthy microbiota produce short-chain fatty acids, such as butyric acid, which can activate the vagus nerve and send messages from the gut to the brain. It is highly beneficial to get most probiotics through diet. However, if supplements are used, it is recommended to use good quality broad-spectrum probiotics.
Download Your Copy!
Meditation
Meditation has been found to increase vagal tone and positive emotions. Meditation for 10-15 minutes is a great way to start the day, manage stress, and stimulate the vagus nerve. There are many ways to meditate and many types of meditations. Mindfulness meditation is the most tested in kidney patients. It has been demonstrated to improve the quality of life, reduce anxiety and depression, reduce sympathetic overactivity,improve sleep, and improve blood pressure.
To practice mindfulness meditation such as Benson’s relaxation technique, follow these steps:
- Sit in a comfortable position or on a meditation cushion.
- Close your eyes.
- Relax your shoulders and muscles.
- Focus on breathing.
- Say a word with every exhalation. A positive word like “gratitude” can be used. As the mind starts racing, which distracts from the breath, the person returns to the word.
Practicing this every day will improve the experience and compound the benefits with consistency.
Omega-3 fatty acids
Among the many benefits of omega-3 fatty acids are increased vagal activity. The best way to reap the benefits of omega-3 fatty acids is by eating fatty fish twice per week, but if that is not an option due to protein restrictions or dietary choices, supplementation is an option. Other food sources include nuts and seeds such as walnuts and flaxseed. It is important that the supplement contains enough eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), which are the most powerful omega-3 fatty acids. The dose is at least 500-1,000 mg of EPA-DHA three times a day.
Exercise
One of the best vagal tone exercises is exercise itself. Exercise is linked to better mental health and stimulation of the vagus nerve. It may be one of the most underutilized yet effective interventions for the prevention and treatment of kidney disease. It has been shown to reduce the risk of CKD, help with blood pressure and glucose control, and improve health-related quality of life. Exercise also induces a positive influence on mental health, mood, and stress levels by stimulating the vagus nerve.
The best type of exercise is the one that you do. What I mean by that is don’t get discouraged by trying to find the perfect type of exercise and do anything that works best for you. Having said that, studies on exercise in CKD have included resistance training and aerobic activities that use large muscle groups continuously such as walking, cycling, and jogging.
High-intensity interval training (HIIT) offers superior benefits in individuals with metabolic diseases such as diabetic kidney disease. Studies of HIIT in CKD have shown that it is a safe and feasible option for individuals with CKD.
Those who are new to exercising should start slowly and gradually get to 20-30 minutes of strenuous exercises 5-6 days a week. It is best to alternate between aerobic exercises and resistance training. For those who are 50 years of age or older, it is important to check with your provider before engaging in strenuous exercises.
Massage therapy
Massage therapy has also been found to be associated with improved vagal tone. The stimulation of pressure receptors leads to an increased vagal activity which, in turn, seems to mediate the diverse benefits of massage therapy. Functional magnetic resonance imaging data suggested that moderate pressure massage was represented in the part of the brain involved in stress and emotion regulation.
Socializing and laughing
Finally, increased social connection and laughing have been linked to increased positive emotions. Increased
positive emotions, in turn, produced increases in vagal tone, which puts the body in a rest and repair state.
The bottom line
Stimulating the vagus nerve can turn on the parasympathetic nervous system, improve renal blood flow, and modulate inflammation in CKD. Improve kidney health using these natural techniques to turn on the vagus nerve and turn off stress: a cold shower, breathing exercises or meditation, singing or humming, probiotics, omega-3 fatty acids, exercise, massage, and social connection. Check out my 1-hour morning routine for kidney health that incorporates many of these techniques.
The post Nine Ways to Naturally Stimulate the Vagus Nerve, Lower Stress, and Promote Kidney Health appeared first on Integrative Kidney.]]>This routine should take no longer than an hour. Your kidneys and health deserve an hour from you every morning. I understand many of us have hectic lives, but if you are busy, try to go to bed early and wake up one hour earlier the next morning. Trust me, it is worth it. An hour morning routine beats dialysis any time. This could be the first step in how to heal your kidneys naturally.

Start with water
At night the body loses a lot of water due to sweat and breathing. In fact, in a small study presented at an Associated Professional Sleep Societies meeting in 2009, healthy young men were found to lose ¼ lbs. per hour while asleep. That is about 2 lbs. in eight hours of sleep.
This is why you should start your day with water. The rest of the routine can be done according to your judgment and comfort. Start with drinking two glasses of filtered water if you are not on any water restrictions. This is even more important for patients with polycystic kidney disease and kidney stones. If you are wondering how much water to drink in PKD, check out our calculator here.
Exercise
Exercise for about 20 minutes. The type and duration of exercise depend on an individual’s level of functioning, endurance, and preference. Studies on exercise in chronic kidney disease (CKD) have included resistance training and aerobic activities that use large muscle groups continuously such as walking, cycling, and jogging.
High-intensity interval training (HIIT) was shown to offer superior benefits in individuals with metabolic disease. In the few studies of HIIT in CKD, it was found to be a safe and feasible option for individuals with CKD.
If you are new to exercising, start slow and try to gradually get to 20 minutes of strenuous exercise five to six days a week. It is best to alternate between aerobic exercise and resistance training. If you absolutely can’t fit exercise into your morning routine, you can move it to whatever time that works for you. The benefits are all the same. Consistency is the key here.
Download Your Copy!
Meditation
Meditate for at least 10 minutes. Meditation is a great way to start your day, manage stress, and stimulate your vagus nerve, which connects the brain with many vital organs including the kidneys. There are many ways to meditate and many types of meditations. Mindfulness meditation is the most tested in kidney patients. It has been shown to improve the quality of life, reduce anxiety and depression, reduce sympathetic overactivity, improve sleep, and improve blood pressure.
To practice mindfulness meditation such as Benson’s relaxation technique, sit in a comfortable position or on a meditation cushion, close your eyes, relax your shoulders and muscles, and focus on your breathing. Say a word with every exhalation. Pick a positive word like “gratitude.” As your mind starts racing to distract you from your breath, try to return to the word you chose. Practicing this every day will make you better at it, and you will be able to reap all the benefits with consistency.
Join us in the fight against kidney disease and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
Journaling
Journaling is a great way to write your thoughts and plan your day. It has similar benefits to meditation. In fact, journaling was found to reduce stress and depression, boost the immune system, and improve memory among many other benefits. You can write whatever comes to mind. Think of it as a thought download. This should also not take more than 10 minutes.
Meditation and journaling can also be moved to a different time of the day for busy individuals with similar benefits. If you are very busy, consider meditation in the morning and journaling in the evening.
Cold shower
Taking a cold shower has many benefits for kidney patients. It increases endorphins and fights off depression, and it improves metabolism and circulation. Most importantly, it stimulates the vagus nerve and improves renal circulation. It may also soothe itchy skin, which is common in CKD patients. Cold showers help with post-workout muscle soreness. The benefits of a cold shower begin when the water temperature dips to 60 degrees Fahrenheit. This is 40 degrees lower than the typical steamy shower.
Now, I know it will be hard to turn that shower knob from hot to cold in the morning. The way to do it is to start with your hot shower. Then gradually lower the temperature at the end of the shower every day by turning the knob to cold. Give your body time to adjust. You can start with 30 seconds under the cold and gradually increase it to a maximum of three minutes. A quick shower for kidney health takes 10 minutes.
Plant-based breakfast
A good plant-based breakfast can be a super healthy way to start your day. A plant-based or plant-dominant diet has been linked to better kidney health and to slow the progression of kidney disease. There are many options that you can prepare in less than 10 minutes or plan the day before. You can find a few recipes in this e-book.
The bottom line
Your kidneys and health deserve an hour from you every morning. This morning routine can improve kidney health and help slow the progression of early kidney disease. If you’re wondering how to heal kidneys, this routine could serve as the first step, or it could be all you need for heathier kidneys. You can modify it to fit your schedule so that you’re at least doing some of the suggested morning actions every day. If you’ve been wondering how to improve kidney function, this morning routine is an important step in the right direction.
The post How To Improve Kidney Function with a Morning Routine appeared first on Integrative Kidney.]]>
By Majd Isreb, MD, FACP, FASN, IFMCP
The nervous system and kidney health
The autonomic nervous system describes the system that controls involuntary actions, such as heartbeat and the widening or narrowing of blood vessels. It has two components: the sympathetic system (fight or flight system), and the parasympathetic system (or the rest and digest system).
It has been long established that the sympathetic system innervates all segments of the kidneys including the blood vessels and tubules. Stimulating the sympathetic system (fight or flight) can affect blood flow to the kidneys and lead to sodium retention at the level of the tubules, resulting in the progression of kidney disease. The kidneys are also innervated by small branches of the parasympathetic (rest and digest) vagus nerve.
What is the vagus nerve?
The vagus nerve is the longest nerve in the body. The word “vagus” means “wanderer” in Latin. This nerve is described as such because it connects the brain with many vital organs including the heart, lungs, gut, liver, spleen, and kidneys. It, therefore, affects breathing, digestion, and heart rate. Early studies also demonstrated that it also affects kidney blood flow.
Fascinating new evidence shows that the vagus nerve plays an important role in modulating inflammation in the body. When foreign particles are identified in various organs, “inflammatory signals” or neural messages are conveyed to the brain by the vagus nerve. The vagus nerve, then, transmits reflex signals back. These signals end up activating the splenic (spleen) nerve, which leads to a decreased inflammatory response and reduced inflammatory cytokines.
Simply put, the vagus nerve identifies triggers for inflammation and helps the brain regulate the inflammatory response. This is an evolving field called the cholinergic anti-inflammatory pathway (CAP).
Download Your Copy!
Stress worsens kidney disease
Our increasingly stressful lives can lead to increased cortisol levels, insulin resistance, and inflammation. Stress has been linked to imbalances between the sympathetic and parasympathetic systems. This is often described as autonomic dysfunction. These imbalances can also lead to the development and progression of kidney disease. Genetics, environment, and nutrition play important roles in augmenting these changes.
Autonomic dysfunction is a common finding in CKD. It is often measured by what is called heart rate variability (HRV).
Join us to end the kidney disease epidemic and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
Heart rate variability as a measure of vagus nerve activity
HRV is simply a measure of the variation in time between each heartbeat. Because this variation is controlled by the autonomic system, HSV can be used to measure changes in this system. The vagus nerve plays an essential role here since it controls heart rate. Therefore, stimulation of the vagus nerve can affect HRV.
HRV can be measured by analyzing a long strip of electrocardiogram (EKG). However, several companies created “apps” and heart rate monitors that can measure it. Unfortunately, the accuracy of these apps and wearable devices is not yet clear. The easiest way to check HRV is to buy a chest strap heart monitor (Polar, Wahoo) and download a free app such as Elite HRV to analyze the data. Chest straps tend to be more accurate than wrist or finger wearables.
Finally, decreased HRV has been linked to bad outcomes in hypertension, systemic inflammation, depression, and CKD. Low HRV can increase the risk of sudden cardiac death. Therefore, there is increasing interest in manipulating heart rate variability by stimulating the vagus nerve.
Activate the vagus nerve to calm inflammation in CKD
Vagus Nerve Stimulation
CKD is a state of chronic inflammation that is associated with heart disease and poor outcomes. As mentioned above, the vagus nerve plays an important role in detecting and calming inflammation in the body. It identifies sources of inflammation and helps the brain modulate the inflammatory response appropriately. The vagus nerve may play an anti-inflammatory role in conditions such as endotoxin-induced sepsis, arthritis, and acute kidney injury.
Electrical stimulation of the vagus nerve is the most common method to modulate the inflammatory response and other functions of the vagus nerve. Pharmacological methods are also being studied for that purpose. However, there are many simple and natural ways to stimulate the vagus nerve.
Natural ways to stimulate the vagus nerve
Stimulating the vagus nerve can improve the response to emotional and physiological stress, thereby improving kidney health. It can also help decrease inflammation. In fact, the FDA approved a surgically implanted device that stimulates the vagus nerve to treat resistant depression. However, there are many ways to stimulate it naturally. I will mention them briefly here.
Activate the Vagus Nerve Naturally to Improve Kidney Disease:
- Cold exposure such as cold showers.
- Deep and slow breathing can activate the parasympathetic system.
- Singing, humming, chanting, and gargling can also activate the vagus nerve because it is connected to the vocal cords.
- Probiotics, interestingly, can be beneficial in activating the gut-brain axis and stimulating the vagus nerve.
- Meditation has been found to increase vagal tone and positive emotions.
- Omega-3 fatty acids have yet another great benefit- increasing vagal activity.
- Exercise is of course linked to better mental health and stimulation of the vagus nerve.
- Massage therapy has also been found to be associated with improved vagal tone.
- Socializing and laughing can also be beneficial.
The Bottom Line
Emotional stress can be associated with faster progression of CKD. The kidneys have both sympathetic and parasympathetic innervation. Acute stress can worsen kidney function, while relaxation practices can promote kidney health. Stimulating the vagus nerve can turn on the parasympathetic nervous system, improving renal blood flow and modulating inflammation in CKD. Stress reduction and the natural stimulation of the vagus nerve can help delay the progression of kidney disease.
The post Natural Treatments to Improve Chronic Kidney Disease: Vagus Nerve Stimulation appeared first on Integrative Kidney.]]> 
There are practical steps that you can take to improve your sleep. These include creating a relaxing sleep environment, lowering the temperature in the bedroom, making sure it is dark, and having a comfortable mattress, etc. Yet, many people don’t realize that a good sleep is more about what we do away from the bed than what we do in bed.
Join us in the fight against kidney disease and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
In the era of social media, technology, and 24-hour news that are always available in the palm of our hands, our minds are going a million miles per hour. Many of us are juggling so many things and have even more worries. We worry about work, about the kids, emails, social media reactions, finances and many other things. Some of us get to bed with exhausted bodies but minds that are still going at full speed.
So, what do you need to do to help the brain shut down? Here are the five steps to help you unwind your brain and get a better sleep.
Step 1: Don’t carry today’s problems into bed
Your mind is not going to stop thinking about today’s problems and worries unless you help it clean up. You must tie up all the loose ends from the day. The best way to do that is by allowing your mind to settle down two hours before bedtime. Simply, write down ALL your thoughts and worries on a paper or in a notebook. It does not matter how or what. Think of it as a thought download or a brain dump.
Do this process outside the bedroom and leave the notebook or paper there. This will train your brain to leave the worrying thoughts outside the bedroom. It allows space for positive thoughts. Positive thoughts are calming and will help you to go to sleep.
Block "fundamentals" not found
Step 2: Plan your tomorrow
After you downloaded your thoughts, look at your plan for the next day. Look at your calendar and prepare for that early meeting, pick workout clothes, prepare and pack for lunch. Your attention to details will help your mind avoid the worry about tomorrow. This will set you up for success and give you control. The control that will help you settle your mind.
Step 3: Keep your phone outside of the bedroom
In fact, keep all electronics out of the bedroom. The bedroom is for two things, sleep and intimacy. I actually recommend that you stop looking at your phone, social media, emails or any other projects for two hours before going to bed. Trust me, I know it is hard and I am guilty of this too.
I also get that some of you may be in a profession like me where you take calls at night and may need a phone nearby. But in the era of smartphones, it is easy for the mind to wander at night. These types of phones bring your worries and the whole world with you to the bedroom. Do you want the world to be in your bedroom when you’re trying to sleep?
So, if your profession requires it, get a landline or cheap flip phone to be by your bed for emergencies. No texting, no social media, and no news in the bedroom. Research found that one third of people wake up at night and check their smartphones.
Step 4: Create a bedtime restorative ritual
A restorative ritual signals your brain that you’re going into a relaxed state. These rituals include things like taking a bath or a hot shower, drinking hot green tea, lighting up candles, dimming the lights, praying or meditating. You can also read a fiction book to take your mind out of your own story into the story of the book.
Step 5: Think happy thoughts
Pick a location of your dreams. If you love to be on the beach in Hawaii or on top of mount Everest immerse yourself in the experience. Feel it, smell it, see it and dream it. Visualize it as if you are living in it. This powerful way will calm your mind and set it up for dreaming. The goal is to feel calm, safe, quiet and “tucked in.”
Bonus: what if you wake up in the middle of the night
Waking up in the middle of the night is not unusual. Researchers found that 31% of people wake up in the middle of the night at least 3 times a week. So, if you wake and you can’t go back to sleep, use the 15 minute rule. If you wake up in the middle of the night and after 15 minutes you don’t drift back into sleep, you should get out of bed. Do not lay there and start thinking about going to sleep. Do not look at the time, do not check your phone, and do not make a cup of coffee.
Get up and go to another room. Sit in a comfortable chair, read that novel, light up a candle. If your mind is racing again. Go back to that piece of paper or notebook and write down your thoughts and worries again. Do not do these things in bed because that will train your mind to associate your bed with wakefulness instead of sleep. When you feel drowsy again, go back to your bed and go to sleep.
The Bottom Line
Here is the trick though, you have to do these steps every night. You may feel like you want to stay up watching a movie on your favorite app or stay on your phone or catch up on a project instead of your bedtime ritual. But your health and your mind deserve a good sleep. So, this simple promise to yourself will help you establish the good habit of sleep and set you up for better health and success.
The post Five Simple Steps to Improve Sleep For Kidney Health appeared first on Integrative Kidney.]]>Polycystic kidney disease (PKD) is the most common inherited kidney disease affecting one in 800 people. There have been several advances in our understanding of PKD since our last blog. In a previous blog, we discussed the genetics of PKD and how genetic variants translate into a disease. In this blog, we will discuss recommendations for water, salt, and caffeine intake to reduce cyst growth. You will find out if ketogenic diet or intermittent fasting is the best diet for polycystic kidney disease.
PKD at the Cellular Level
To determine the best PKD diet and lifestyle recommendations, we must understand what is happening at the cellular level. In essence, abnormalities in PC1 or PC2 proteins will activate two pathways inside the cell. First, it activates the cAMP pathway which regulates fluid transport. Second, it changes the way cells make energy from sugar (called glycolysis). When PC1 or PC2 proteins don’t work well, they switch from aerobic (with oxygen) to anaerobic (without oxygen) glycolysis. This is similar to the shift that occurs in cancer cells.
While anaerobic glycolysis produces less energy from glucose, it is faster than aerobic glycolysis. This faster energy production allows the cells to grow faster. However, it also leads to a critical dependence on glucose.1
How Much Water to Drink in PKD
Vasopressin, also called anti-diuretic hormone (ADH), is a hormone that is produced by the brain and excreted by the pituitary gland. It plays an important role in the body’s fluid and sodium balance, blood pressure, and kidney function. ADH was found in several studies to promote cyst growth by stimulating the production of cAMP. Further proving the role of ADH in polycystic kidney disease, cyst growth was inhibited in both forms of PKD by administering ADH receptor blockers (medications that block ADH).
Dehydration can increase ADH and make cysts worse. Drinking large amounts of water leads to a significant decrease in the progression of PKD. The optimal amount of water to drink in PKD patients depends on the amount of salt and food they eat. The simplest way to assess this is by checking a 24-hour urine osmolality. You can use our calculator to assess the amount of water you should drink daily based on your 24-hour urine osmolality. Alternatively, measuring first morning urine osmolality can be used. The target for that is keeping the level less than 280 mOsm/kg.
In addition to dehydration, other factors that lead to the production of ADH include stress, pain, and surgery. These factors, therefore, can indirectly lead to cyst growth and further harm kidney function.
Download Your Copy!
Polycystic Kidney Disease and Caffeine
In the laboratory, caffeine increased cAMP accumulation in the cells. Yet, in human clinical trials, caffeine intake was not directly associated with kidney size in patients with PKD. An analysis in one clinical trial found no significant association between the consumption of caffeine from coffee and tea on the progression of ADPKD.
Join us in the fight against kidney disease and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
Calorie-restricted and Keto Diets for Polycystic Kidney Disease
Kidney cysts thrive on sugar or glucose, as discussed earlier. Therefore, calorie-restricted and ketogenic diets can be beneficial for patients with PKD. Ketogenic diets induce a state that resembles starvation by providing high fat content and low protein and carbohydrate content. Time-restricted feeding such as intermittent fasting can have similar effects. Studies on animals demonstrated that ketosis could decrease cyst growth in PKD. These effects were thought to be mediated by a strong inhibition of mTOR.2
It is worth mentioning here that metformin can activate AMPK and is currently being studied in PKD.
To our knowledge, there is no published human study to confirm the effect of ketogenic diets and intermittent fasting on PKD. However, given the strong benefit of ketosis on cyst growth, we generally recommend a plant-based ketogenic diet or intermittent fasting in addition to a large water intake for patients with PKD.
Dietary, Lifestyle, and Water Recommendations for PKD
The phrase “our genes are not our destiny” describes how nutrition and lifestyle factors can have a positive impact on genetic expression for certain diseases. Drinking large amounts of filtered water, restricting salt intake, a ketogenic diet, or intermittent fasting can have significant benefits in patients with PKD. So far, limiting caffeine is not necessary to improve PKD, but it has other health benefits. Finally, stress reduction techniques can help to lower ADH and reduce kidney cysts.
Ongoing Studies of Diet and Lifestyle PKD Treatments
- PREVENT-ADPKD trial is looking at water intake and the progression of ADPKD. It should be released in late 2021.
- DRINK trial is investigating water intake in ADPKD. It should also be released in late 2021 or early 2022.
- METROPOLIS trial is comparing Metformin and Tolvaptan for the treatment of ADPKD. It should be completed in early 2022.
- Time-restricted feeding in ADPKD is currently recruiting subjects and is estimated to be completed by end of 2022.
- Keto-ADPKD trial is looking at how the ketogenic diet affects the progression of ADPKD. It should be completed in mid-2022.
- Curcumin Therapy to treat vascular dysfunction in ADPKD was completed in late 2020. It should be released soon.
1 It is noteworthy that glycolysis is inhibited by a cellular messenger called AMP-activated protein kinase (AMPK). It is activated by another messenger called mTOR. Metformin activates AMPK.
2 Activation of AMPK and inhibition of mTOR can theoretically inhibit glycolysis in cells that line the cysts in PKD. However, studies that looked at medications that inhibit mTOR such as sirolimus, did not show any benefit in PKD.
The post Diet and Lifestyle Modifications in PKD appeared first on Integrative Kidney.]]>
Types of Stress
Generally speaking, there are three types of stress:
- Major catastrophic life events that require considerable behavioral modification such as the death of a loved one, divorce or loss of a job.
- Chronic strains that are persistent stressors which require some adjustment over a long period of time such as poverty or disability.
- Daily hassles that occur over the course of the day such as traffic issues or unpleasant personal interactions.
The way people perceive and handle stress varies from person to person, with some people better equipped to handle stress than others. Certain factors, which we detail below, impact a person’s ability to cope with stress. These include genetics, environment, and in utero exposure. Furthermore, previous traumatic life experiences may affect future handling of stress in an individual.
Most of the early literature on stress focused on the first two types listed above, but research is now looking at the third type and its effect on health.
According to Selye, there are three phases of behavioral adjustments to stressors. The first phase is the alarm stage in which a person will have a “fight or flight” response. If the stressor persists, the person enters into the resistance or adaptation stage. Finally, long term exposure to the stressor will eventually lead to the exhaustion stage.
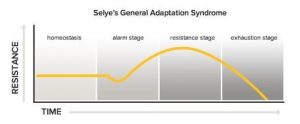
Factors that influence stress
Although we all experience stress, some individuals are better suited to handle stress than others. There may be some individual variability due to various genetic and environmental factors, as well as the impact of trauma and adverse childhood experiences.
Genetics
Small differences in our genes, called single nucleotide polymorphisms (SNPs), can affect our hormonal responses and enzymes that are associated with psychological responses. One example is a SNP in catechol-O-methyltransferase (COMT) gene which produces an enzyme that breaks down dopamine, epinephrine, and norepinephrine (neurotransmitters associated with the fight-or-flight response). Mutations in the way this gene is expressed, can lead to an increased stress response.
Another example is a protein called brain-derived neurotrophic factor (BDNF) which protects and improves signaling between brain cells. Any SNPs in BDNF or its receptors can decrease resilience to stress. In fact, the impact of stress on BDNF has been strongly associated with affective disorders.
Environment
The area and physical environment where a person lives and works can be a stressor. Environmental stressors such as living in disadvantaged neighborhoods, limited access to supermarkets, residential density, availability of recreational resources, and distance to wealthy areas, are associated with the development of insulin resistance, type 2 diabetes, obesity, and cardiovascular disease, all of which are risk factors for CKD. It is important to know this is subjective and environmental stressors for one individual may not be stressful to another.
In Utero Exposure
The stress a woman experiences during pregnancy can greatly impact the development of the baby while in utero, leading to lifelong complications. Prenatal stress has been shown to affect hypothalamic-pituitary-adrenal (HPA) axis programming of the fetus, making it more difficult for the offspring to handle stress in the future. Furthermore, this altered HPA activity has been linked to low birth weight which may result in a decrease in nephron endowment (the number of filtering units the baby is born with), as well as metabolic syndrome and cardiovascular disease, known risk factors for CKD.
Nutrition as a Stress Mediator
Research suggests that some nutrients can heighten the response to stressors while other nutrients relieve it. For example, magnesium and zinc can help a person feel more calm. In addition, omega-3 fatty acids and foods high in probiotics can reduce stress and anxiety. On the other hand, caffeine can make a person feel anxious. It is important to note that genetics play a role in caffeine metabolism and its effects.
Indirect Effect of Stress on the Kidney
Stressors can lead to changes in the hypothalamic-pituitary-adrenal axis (HPA axis) and neuroendocrine hormones. These changes are associated with increased cortisol levels, increased epinephrine, and inflammatory cytokines which are linked to the development of insulin resistance, metabolic syndrome, high blood pressure and type 2 diabetes.
Direct Effect of Stress on the Kidney
Studies have shown that the sympathetic system innervates all segments of the kidneys including the blood vessels and tubules. Stimulating the sympathetic system can affect blood flow to the kidneys and lead to sodium retention at the level of the tubules, resulting in the progression of kidney disease.
The Vicious Cycle
As we have seen above, epinephrine and norepinephrine can play a role in the psychological stress response on the kidneys. These neurotransmitters are usually broken down in our bodies by two major enzymes: monoamine oxidase (MAO) and COMT. Recently, a new enzyme, renalase, was found to be produced by the kidneys and involved in the breakdown of these neurotransmitters.
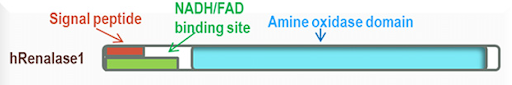
Renalase is a flavoprotein that metabolizes catecholamines (epinephrine, norepinephrine, and others) to aminochromes. It utilizes NADH as a cofactor. Therefore, deficiencies in vitamin B2 and B3 can affect its function. Studies have shown that renalase levels in the blood correlate with normal kidney function and kidney mass. Decreased level of renalase leads to elevated blood pressure and heart rate, physiological responses to stress. Furthermore, it’s been shown that decreased levels of renalase increase the sensitivity of the heart and the kidneys to ischemia (decreased blood flow).
This creates a vicious cycle in which stress causes kidney disease and the latter, in turn, amplifies the effect of stress on the body.
In essence, the interplay between stress and kidney disease can be summarized in this diagram.
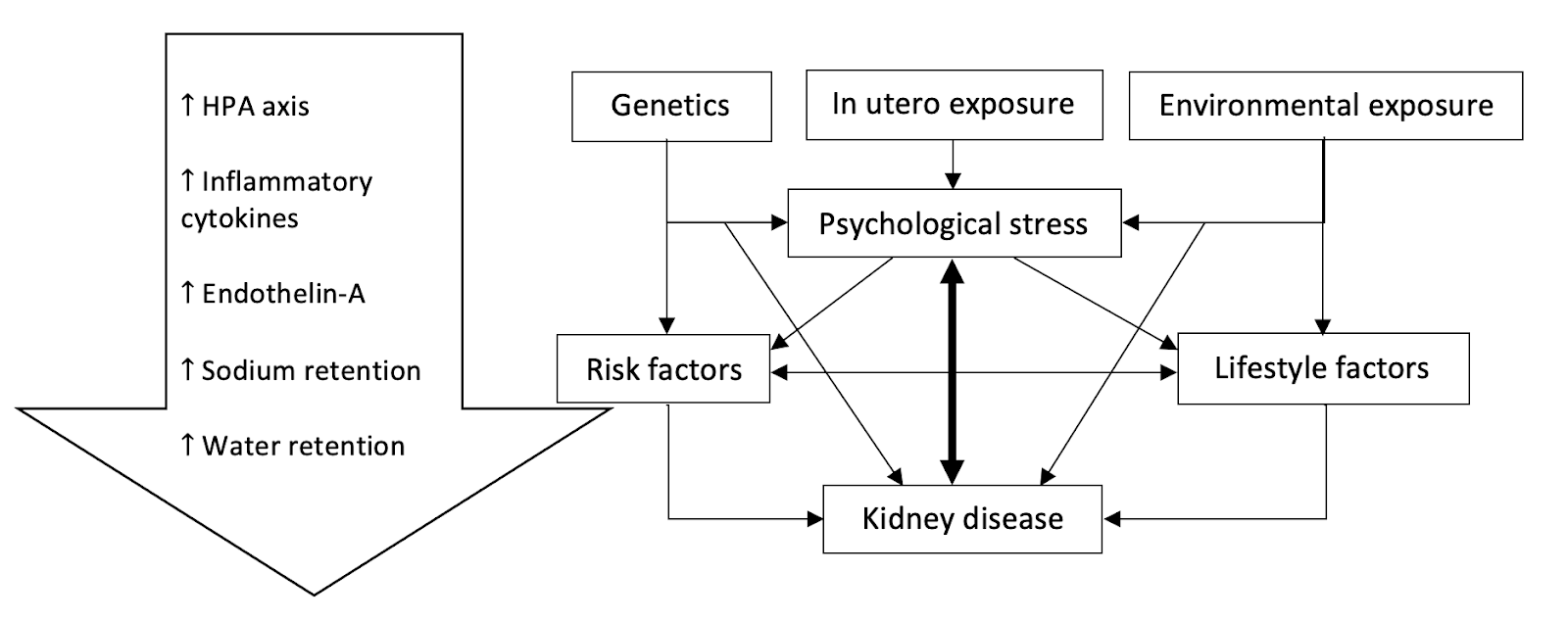
The Bottom Line
Our increasingly stressful lives can lead to increased cortisol levels, insulin resistance, and inflammation. Stress has been linked to increased levels of epinephrine and norepinephrine. These changes lead to the development and progression of kidney disease. Genetics, environment, and nutrition all play important roles in augmenting these changes. It’s essential that a stress management practice is part of a comprehensive Integrative and Functional Medicine approach to kidney health.
The post Stress and kidney health appeared first on Integrative Kidney.]]>

Exercise may be one of the most underutilized yet effective interventions for the prevention and treatment of chronic disease. It has been shown to reduce the risk of complex chronic disease, help with blood pressure and glucose control and improve health-related quality of life. Other benefits of exercise include positive influence on mental health, mood and stress levels, important factors to overall health and wellness. In this blog, we will discuss the benefits of exercise in kidney health.
By Megan Morrison, PharmD
The implications of kidney disease are vast. It is an extremely costly disease, with many people progressing to end stage renal disease (ESRD) requiring dialysis or a kidney transplant, a significant physical and financial burden. Often the disease dramatically reduces an individual’s quality of life, the ability to perform activities of daily living, and independence.
Furthermore, kidney disease is associated with a high symptom burden, cardiovascular disease and increased mortality rates. With the prevalence of chronic kidney disease (CKD) on the rise, along with diabetes and hypertension, it’s imperative that prevention and an integrative medicine approach to kidney health become the norm along with exercise, a modifiable lifestyle factor.
Benefits of exercise in kidney disease
Physical inactivity is associated with a decline in kidney function in CKD. Exercise has the ability to markedly improve numerous health parameters associated with the disease, including:
- Cardiovascular health
- Systemic inflammation
- Muscle mass
- Gut health
- Mortality rate
- Risk factors associated with CKD, including diabetes and high blood pressure.
Exercise improves cardiovascular health and vascular function
Patients with CKD have an increased risk of cardiovascular disease (CVD). In fact, rates are estimated to be 10-20 times higher among ESRD patients than the general population. High blood pressure, the second leading cause of kidney failure in the US after diabetes, is closely related to adverse kidney and cardiovascular outcomes in CKD. This is why reducing blood pressure is imperative.
Benefits of exercise on blood pressure management are well-established. One study in pre-dialysis patients showed reductions in both systolic and diastolic blood pressure in participants who engaged in 1-hour of acute aerobic exercise such as walking. Another study found that 1 hour of supervised, home-based exercise reduced arterial stiffness over 3-months and improved outcomes in pre-dialysis patients.
Exercise positively effects inflammatory markers
Chronic inflammation has detrimental effects on health and is associated with increased cardiovascular events, the leading reason for mortality in CKD. Plasma inflammatory markers have been found to be positively affected by exercise. A study found that a 30-minute bout of exercise increased plasma IL-10 levels and regular walking 5 days a week for 6 months reduced the plasma IL-6:IL-10 ratio favorably. IL-10 is an anti-inflammatory cytokine, while IL-6 is inflammatory. The reduction in the IL-6:IL-10 ratio seen in the regular exercisers reflects a decrease in overall inflammation.
Exercise increases muscle mass
Muscle wasting, which promotes a sedentary lifestyle and increases morbidity and mortality, is another complication associated with CKD. An 8-week resistance training program (3 times a week) for pre-dialysis patients increased muscle mass, with similar findings in dialysis and transplant patients.
Exercise favorably impacts the gut microbiome
In a previous blog post, we discussed the close relationship between the quality of the microbiome and the health of the kidney, known as the gut-kidney axis. Those with a healthy microbiome balance, defined as an abundance of “good” bacteria, and the absence of pathogenic species or overgrowth, are less likely to develop CKD.
One study that compared active women and sedentary controls found that women who performed at least 3 hours of exercise per week had increased levels of beneficial bacteria. Additional studies have shown that exercise increases fecal butyrate concentrations and the relative abundance of butyrate-producing taxa. Butyrate is a short-chain fatty acid produced by bacteria that positively impacts intestinal health by supporting a favorable environment for commensal growth.
Exercise significantly reduces mortality rate in ESRD
ESRD is associated with considerable morbidity and mortality. A study of dialysis patients found that those who regularly exercised (2-5 times per week) had significantly lower all-cause and cardiovascular mortality rates than less active peers.
Type and Duration of Exercise
The type and duration of exercise depends on an individual’s level of functioning, endurance, and preference. Studies on exercise in CKD have included resistance training and aerobic activities that use large muscle groups continuously such as walking, cycling, and jogging. High-intensity interval training (HIIT), which has gained popularity in recent years, has shown to offer superior benefits in individuals with metabolic disease. In the few studies of HIIT in CKD, HIIT was found to be a safe and feasible option for individuals with CKD, including those undergoing hemodialysis. Regardless of type, duration, or intensity, regular exercise is beneficial in CKD patients.
Considerations & Contraindications
Individuals with CKD should consult their healthcare provider before beginning any type of new exercise routine. Certain subgroups of the CKD population need special considerations including those with known or suspected cardiac disease and dialysis patients.
It’s important to note that patients with kidney disease have identified certain barriers to exercise which include fear of injury or aggravating their condition, poor physical condition as a result of both co-morbid conditions and CKD-related symptoms, a lack of guidance from health professionals, and a lack of facilities and social support. Exercise facilities are less defined and less accessible to the CKD population in comparison to services provided for cardiac and pulmonary patients, resulting in fewer opportunities to develop peer support groups, which can significantly effect exercise adherence. It is our responsibility as integrative clinicians to discuss exercise with patients and include physical therapists and trainers in our protocols for management of CKD.
The Bottom Line
The majority of risk factors for CKD are related to lifestyle factors or conditions related to lifestyle disease. Exercise is an intervention that has the ability to positively impact a large number of those risk factors. Integrative and Functional Medicine prioritizes the vital role that physical activity plays in overall health and wellbeing, including exercise as part of the holistic therapeutic plan. There are benefits to any level of exercise, it’s important to guide patients to choose activities that are safe, meet them where they are, are appropriate to their level of physical activity, and are enjoyable.
The post The Many Benefits of Exercise for CKD appeared first on Integrative Kidney.]]>
By Megan Morrison, PharmD
Yoga and meditation are both considered mind-body interventions which the National Center for Complementary and Integrative Health defines as “a range of procedures or techniques focusing primarily on the connections between the mind, body and behavior and their resultant effects on one’s health”.
Yoga, which is said to have originated in India more than 5,000 years ago, literally means “union” and is a practice that aims to balance and harmonize the mind, body, and emotions. Various styles of yoga include regulated breathing techniques (pranayama), physical postures (asanas), hand gestures (mudras), yogic relaxation (yoga nidra), and more. Meditation encompasses several techniques that are used to influence the mind through mechanisms in the parasympathetic nervous system to bring about calm and relaxation.
Both yoga and meditation have been documented to have measurable positive impact on various chronic conditions, including type 2 diabetes and hypertension, two disease states that are major risk factors for the development of kidney disease. We’ll look at the research supporting the benefits of both for kidney health.
Block "fundamentals" not found
Benefits of Yoga for Kidney Health
One study looked at the effects of a 6-month yoga program on renal function and quality of life in patients with chronic kidney disease. After 6 months, the yoga group saw a significant reduction in systolic and diastolic blood pressure, blood urea and serum creatinine levels, and significant improvement in quality of life. Furthermore, subjects in the yoga group had reduced need for dialysis than the control group although not statistically significant.
Another study looked at the effects of a 12-week yoga-based exercise program in hemodialysis patients. Significant improvements were seen for many of the variables measured including pain, fatigue, sleep disturbance, along with significant reductions in creatinine, blood urea, alkaline phosphatase, cholesterol, erythrocyte and hematocrit count.
Although the exact mechanism for many of the benefits of yoga have not been completely understood, they include:
- Improved blood pressure control
- Improved glycemic control
- More regulated eating patterns
- Improvement in markers for kidney function
- Significant reduction of the waste products associated with kidney damage, urea and serum creatinine
- Improved physical and psychological quality of life for kidney patients on dialysis
- Improved blood supply to muscles and increased muscle activity, strength, endurance, flexibility, and balance
- Favorable effects on body weight, adiposity, dyslipidemia, and insulin resistance
- Significant reduction in oxidative stress and increased antioxidant activity
- Improved parasympathetic tone, helping offset fight-or-flight response often associated with chronic disease
- Reduced need for dialysis
Benefits of Meditation for Kidney Health
In a study of 15 African American males with CKD and high blood pressure, there was a significantly greater reduction in systolic and diastolic blood pressures, mean arterial pressure, heart rate, and muscle sympathetic nerve activity during mindfulness meditation compared with the control.
Those with end-stage renal disease as well as mild CKD have been shown in multiple studies to have chronic activation and elevation of the sympathetic nervous system (SNS). Therefore, using a non-invasive, safe therapeutic intervention such as meditation to lower SNS activity in those with renal disease may mitigate long-term consequences.
One type of mindfulness meditation technique studied in kidney patients is called Benson’s relaxation technique which consists of “eye closing, muscle relaxation, breathing awareness, breathing out stating a word, and returning to the “word” when participants’ thoughts are distracted”. This technique has been shown to reduce levels of anxiety, depression, and improve sleep quality as well as improve quality of life in patients undergoing hemodialysis.
Benefits of meditation for those with kidney disease include:
- Improved quality of life for hemodialysis patients
- Reduced anxiety and depression
- Reduced sympathetic overactivity
- Better sleep
- Reduced blood pressure
- Less prone to various forms of stress
The Bottom Line
Research has demonstrated that yoga and meditation greatly improve measurable health outcomes and quality of life in those with kidney disease or those looking to protect their kidney health. Both modalities are generally safe for most people, but it’s best to consult your physician before initiating any exercise program including a yoga routine. When working with a clinician trained in Integrative or Functional Medicine, they will often suggest incorporating some type of mind-body intervention as part of your holistic therapeutic plan.
The post Yoga and Meditation for Kidney Health appeared first on Integrative Kidney.]]>
The root causes of my sleep problems go far back, with mild symptoms of pregnancy insomnia in my third trimester. After giving birth, I became an extremely light sleeper who could be awakened by hearing anyone tiptoeing nearby. I became hyper-vigilant. I thought it was driven by me being a new mom. I was getting up multiple times through the night to heed to my newborn baby, and then staying wide awake the rest of the night. However, that chronotype of light sleeping continued throughout the following years.
My journey with suboptimal sleep.
In 2016, when I was a victim of a chronic job, I was drained by a huge workload and long hours. I was assailed with onerous functional, technical, and humanitarian ethical commitments. My job required crossing several time zones. My social life was badly affected and my social circle narrowed significantly. I was severely sleep deprived, barely getting 2-3 hours a night for days in a row and occasionally getting 5 hours once in a blue moon.
In the beginning, I didn’t feel the negative effects of poor sleep. I was getting up early in the morning feeling energetic, motivated, and looking forward to my day as if I had good sleep the night before. That made me wrongly think that I might be blessed; my body doesn’t need long hours of sleep for me to be able to fully function. Having the extra hours in my day seemed to help me perform at a high level, deliver more, and enjoy my time.
Consequently, I stopped obsessing about getting enough sleep and started to adjust to my insomnia, telling myself I’m lucky that I’m unfettered and not wasting my time with unnecessary sleep. When I was in bed trying to sleep every night, my brain was hyper alert; I was not able to stop the thoughts circulating in my mind, and when I awoke in the morning, I felt like my brain had been racing while I was sleeping.
The fatigue began to catch up, causing my mental and emotional state to shake. I was gradually running out of energy. Any energy I did have to socialize or practice my hobbies was diminishing day by day. The fatigue also stirred my vitality and my mood disorder was on the rise.
I started to look for remedies to beat my sleep disorder. I tried melatonin supplements, sought advice from sleep therapists, heard about acupuncture, listened to alpha waves tones, drank herbal tea and had amber/rose aromatic baths pre- bedtime. The last thing I tried was based on advice from a colleague of mine, who recommended that I wipe my eyes with the water of soaked jasmine petals so that I could fall asleep.
Unfortunately, none of these worked for me.
Deep dive into our brain circuits.
As a science-oriented person, I was interested in decoding the chemistry of the brain and the Cognitive Neuroscience of Sleep to understand how to use neuroscience to improve my sleep and how stress and worrying affect sleep. I learned that my daily routine, along with managing my reaction to stress, can change the activity of the neurotransmitter systems in my brain, and can therefore positively impact my insomnia. I read the article published on InKidney titled “Sleep and Kidney Health”, in addition to the book The Upward Spiral by Alex Korb, PhD which helped me understand the biological basis of sleep disorders and adopt practical tips to improve my sleep cycle. One caveat of the aforementioned book is that it focuses more on how to get out of the downward spiral of depression; thankfully, I was not suffering from any course of depression. The book also illustrated how the circuits inside our brains are connected to each other (for example, the changes to my daily routine that reduced stress levels, improved mood, and provided me more energy to exercise, significantly contributed to the improvement of my sleep circuit by releasing more norepinephrine, oxytocin, endocannabinoids, dopamine, and melatonin).
The magic of sleep.
To improve sleep, we must first understand what I call “the magic of sleep.” I became familiar with the sleep architecture of our brains. That was key to understanding the stages of sleep and the governance the brain has on hormones/neurotransmitters and quality of sleep cycle. The circadian rhythm, controlled by the hypothalamus, also plays a role . The hypothalamus governs a large number of our daily activities including hunger, alertness, and body temperature. It also made me aware of the fact that circadian rhythms cause a variety of daily neuro-hormone fluctuations, including melatonin which helps with falling asleep. This biological system can be restored and maintained by sticking to a sleep schedule and making small changes like minimizing light exposure at night.
Figure 1: The Cycle of Melatonin- (Matthew Walker, 2017)
Figure 2: Sleep Architecture- when experts chart sleep on a hypnogram, the different levels resemble a drawing of a city skyline. This pattern is known as sleep architecture. The hypnogram above shows a typical night’s sleep of a healthy young adult.
(the editors of Harvard Health Publishing in consultation with Lawrence Epstein & Program Director, 2019)
Optimizing my sleep hygiene.
Because habits are triggered by stress, I have come to understand the fundamental importance of controlling stress and anxiety. Additionally, I’ve followed a number of tips and strategies that made me feel an immediate lift in the quality and duration of my sleep. The tips to improve sleep are summarized as follows:
Day-time activities:
- Exercise, which is a great part of my daily life, gives me an enormous sense of well-being, and makes me more energetic and positive throughout the day. This translates to more productivity, happiness, and relaxation when I go to bed at night.
- Consume high prana foods (green, organic, whole and unprocessed food) that are energy giving, and necessary to function with the highest levels of productivity.
- Practice mediation for 10 minutes on a daily basis.
- Avoid naps during the daytime.
- Accomplish harder tasks during the daytime only, and keep easier or funnier tasks to the evening time.
- Caring for the people I love which is a powerful pathway to my personal growth, long lasting happiness, and stress relief.
- Self-care, maintain work-life balance, and make time for friends and people I care about.
Pre-bedtime routine:
- Go to sleep and wake up at the same time all days of the week (including weekends). It’s okay to deviate a little occasionally, but there should be a defined target for your sleep and wake up times.
- Refrain from caffeine intake (coffee or tea) 6-8 hours before bedtime.
- No eating after 8:00 PM.
- Lower all lights by a certain time at night.
- Set phone and PC on night-mode, and reduce the brightness on my devices’ screens.
- Stop the use of electronic devices at least 30 minutes before going to sleep.
- Turn off the TV in my bedroom as well as all electronics that might illuminate the room.
- Maintain self-care, healthy diet, and proper hydration.
Bedtime setting:
- Adjust LST (no light, no sound, low temperature).
- Wear light and comfortable sleepwear; sleep on breathable fresh bedding .
- Make my bed my haven; avoid reading or working in bed to associate the bed only with sleep.
- Charge phone away from bed
Wake up routine to stay energized:
- Start the morning with proper hydration and stretching exercises.
- After a warm shower, shower with cold water for up to 5 minutes.
- Journaling and setting the daily highlights.
The Bottom Line
One of the key pillars for building a healthy foundation for good sleep is implementing daytime habits that support a solid nighttime routine. By controlling stress and following the tips above, I have managed to improve my sleep from an average of 3 interrupted hours of sleep into continuous 6 hours of sleep. I’m waking up happier, more put together, more productive, and, most importantly, healthier. I continue to strive for 8 hours of quality sleep. I would like to end with a quote from Dr. Mathew Walker in his book Why We Sleep: “the best bridge between despair and hope is a good night’s sleep”.
Read the bio of Rania M. AlQenneh here.
The post How I Managed to Improve my Sleep appeared first on Integrative Kidney.]]>