Five questions kidney patients should ask before taking a new medication
By Majd Isreb, MD, FACP, FASN, IFMCP
Is it necessary?
There are many instances when a medication may be inappropriate—for example, using an antibiotic for a viral infection. However, with the short time providers spend with their patients, it is not uncommon to see medication being prescribed before any attempt at lifestyle modifications. Lifestyle modifications should be the first step in the management of many chronic diseases. This includes educating patients and coaching them on these modifications for at least six months.
Does it harm the kidneys?
Many medications can cause direct or indirect harm to the kidneys, and every day there is a newer medication on the market. Sadly, some providers may not be aware if a drug being prescribed is harmful to the kidneys or not. It is, therefore, necessary for the patient to ask themselves and their provider that question.
The following table shows a list of common medications and how they may negatively affect the kidneys. This is not an exhaustive list and should be used in consultation with the provider or the nephrologist.
It is also important to remember that some medications commonly used for kidney patients can be harmful in certain situations. For example, a diuretic (water pill) can become dangerous if the patient is not eating or drinking well.
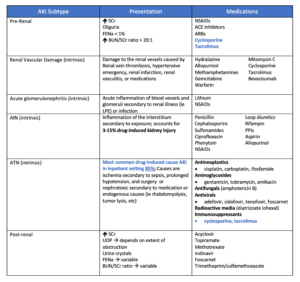
Courtesy: Lara Zakaria, PharmD CNS CDN IFMCP
Should the dose be adjusted to kidney function?
Many of the prescribed medications are excreted by the kidneys. Therefore, the doses of these medications should be adjusted according to the level of kidney function to avoid toxicity or side effects. Some medicines should be entirely discontinued at the advanced stage of kidney disease. This website can be accessed to see the dose adjustment needed for a specific drug according to the kidney function.
Does it interact with other medications?
Drugs can interact with each other in various ways. For example, a medication can affect the absorption of others by the gut. It may affect the way another drug is transported in the circulation. It may decrease or increase its breakdown by the liver or other organs. It can also affect its excretion by the kidneys or the gut. This interaction checker is a valuable tool for providers and patients to see if a drug that is being prescribed interacts with another one that the patient is already taking.
Does it affect micronutrients?
Micronutrients are essential for every structure and function in the human body, including but not limited to the function of the heart, blood vessels, and immune system. Thousands of enzymes in the body require micronutrients for optimal function. Some medications interact with micronutrients, and micronutrients may interfere with the action of drugs. The is a field of study called Drug-Induced Nutrient Depletion (DIND), and many books are written about it. The following table summarizes some of kidney patients’ most commonly used medications with their nutrient interactions.
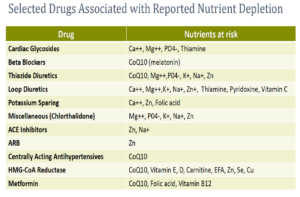
The bottom line
Before taking a new medication, kidney patient should ask themselves and their provider the following questions: Is it necessary? Does it harm the kidneys? Does it interact with my other medications? Should the dose be adjusted for my kidney function? Does it interact with micronutrients? Please do not change or stop your medications without checking with your provider or nephrologist.
Download Your Copy!
The post Five questions kidney patients should ask before taking a new medication appeared first on Integrative Kidney.]]>
By Majd Isreb, MD, FACP, FASN, IFMCP
What is MHR and Why Is It Important in CKD?
Monocytes are immune cells involved in the response to chronic or acute infection, especially from bacteria, fungi, viruses, or protozoa. Activated monocytes release circulating pro-inflammatory cytokines that contribute to systemic inflammation.
On the other side of the equation, HDL, or the “good cholesterol,” is thought to have anti-inflammatory, antioxidant, and anti-thrombotic effects. With the MHR ratio, we are looking at monocytes divided by HDL. Therefore, a higher MHR ratio can be thought of as an inflammatory marker, indicating the presence of systemic inflammation. The MHR ratio is easy to measure and can help you assess the burden of inflammation in CKD.
What is monocyte-to-HDL ratio?
MHR can be simply measured from a complete blood count (CBC) and conventional fasting lipid panel. Then it can be calculated by dividing the absolute monocyte counts (× 106/L) by HDL-C (mg/dL).
Several studies have linked Elevated MHR to systemic inflammation and oxidative stress. Inflammation is also a characteristic of CKD, as discussed here. Oxidative stress is an imbalance between antioxidants and free radicals and maybe a root cause of heart disease, Alzheimer’s, Parkinson’s, chronic kidney disease, and many more. MHR has been found to be associated with carotid intima-media thickness, obesity, and poor cardiac outcomes. It was found to be higher in smokers and those with vitamin D deficiency. MHR levels could also be associated with chronic kidney disease symptoms.
What is the normal MHR value?
I have not seen an agreed-upon value for MHR. However, this study showed that the value in non-smokers was 8.5-14.6. The control group in this study evaluating the association between obstructive sleep apnea and MHR had a value of 9.2 ± 2.6. It is important to note that some studies used logarithmic MHR in their reporting. Until MHR is standardized, we cannot reliably assume a normal value. However, it is safe to say that a ratio above 12 is high and may indicate inflammation.
What does MHR have to do with kidney disease?
MHR was found to be negatively correlated with the estimated glomerular filtration rate (eGFR). MHR, therefore, gets higher with worsening kidney function and is a marker for the relationship between inflammation and CKD. This is consistent with the notion that kidney disease is an inflammatory disorder. Higher MHR was also associated with worse cardiac outcomes in kidney patients.
In addition, MHR predicted the severity of proteinuria (abnormal protein in the urine) and kidney function in patients with primary nephrotic syndrome (such as membranous nephropathy, focal segmental glomerulosclerosis (FSGS), membranoproliferative glomerulonephritis (MPGN), and IgA nephropathy). So, the higher the MHR, the worse the kidney function and proteinuria. This will likely translate into a faster progression of kidney disease. A fascinating new study found a significant association between indole-3-acetic acid and MHR. Indole-3-acetic acid is a gut-derived uremic toxin. It comes from the gut microbiome and accumulates in the body of individuals with kidney disease.
The bottom line on MHR and chronic kidney disease
MHR is a novel marker that can help assess inflammation in CKD and oxidative stress. Measurements are affordable, part of routine lab work, and easy to calculate. Higher values are associated with worsening kidney function, CKD symptoms, and poor cardiac outcomes, so it is worth obtaining this measurement.
Download Your Copy!

What is CoQ10?
CoQ10 is an essential part of the electron transport chain in the mitochondria. It is, therefore, crucial for energy production in the cells. It is abundant in the most metabolically active tissues, which include the heart, kidney, and liver. In fact, the concentration of CoQ10 in the kidneys is second only to the amount found in heart muscle. Deficiency in CoQ10 leads to insufficient electron transport, which leads to increased formation of reactive oxygen species (aka, oxidative stress). The body needs a certain amount of oxidative stress, but too much of it is harmful and is caused by an imbalance between free radicals and antioxidants. There are many other functions for CoQ10, but we will not have room to discuss them here.
CoQ10 and Kidneys: Why the Kidneys Need CoQ10
The kidneys filter waste products from the blood in two stages. The first involves the straining of a large amount of fluid through tiny blood vessels, called glomeruli. However, if the body does not reclaim most of that fluid (known as filtrate), the person will die of dehydration within a few hours. This is why the second stage is so important. In it, millions of tiny tubes in the kidney, called tubules, reclaim most of that filtrate.
About 90% of this retrieval process occurs in the first part of the kidney tubule, which is called the proximal tubule. The proximal tubules are also the site of excretion of many organic substances, medications, and uremic toxins. This process of retrieval and excretion by kidney cells requires a significant amount of energy, or ATP (adenosine triphosphate). This explains why the proximal tubules are so rich in mitochondria and CoQ10. Mitochondria are the powerhouses of the cells, and they manufacture the body’s energy currency, ATP.
Join us in the fight against kidney disease and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
CoQ10 and Kidney Disease
A number of studies investigated CoQ10 and chronic kidney disease (CKD). In a small study of CoQ10 and kidney health from Comenius University Medical Center in Slovakia, plasma concentrations of CoQ10 were found to be decreased in patients with kidney disease. Despite that there was an obvious decrease in CoQ10 levels with decreasing kidney function in that study, it did not reach statistical significance due to the small number of patients tested. The author concluded that oxidative stress occurs very early in kidney disease. Decreased CoQ10 levels in CKD were also confirmed in another study. It also appears that the presence of hypertension worsens CoQ10 deficiency in CKD. In addition, our ability to produce CoQ10 internally decreases with aging.
Medications that deplete CoQ10
Several medications can lower the levels of CoQ10 in the body and these include:
- Statin drugs for cholesterol
- Fibric acid drugs for cholesterol
- Beta-blockers for high blood pressure
- Anti-depressant drugs such as amitriptyline
- Warfarin, a blood thinner
- Certain chemotherapy and HIV medications
Can CoQ10 Improve Kidney Function?
As mentioned above, the kidneys require a lot of energy production. The tubules are very sensitive to oxidative stress, which is common in kidney disease. Add to that the deficiency of CoQ10 that is noted in kidney disease. This makes CoQ10 a very attractive supplement to improve energy production and decrease oxidative stress in the kidneys.
There have been many studies evaluating the role of CoQ10 in CKD. CoQ10 was found to reduce total and LDL cholesterol in kidney patients. It was also found to decrease oxidative stress (by lowering malondialdehyde, a marker of oxidative stress).
Additionally, CoQ10 was found to improve blood pressure control. A CoQ10 dose of 200 mg daily was found to decrease systolic blood pressure by 11 mmHg and diastolic blood pressure by 7 mmHg. This was thought to be due to its improvement in nitric oxide balance leading to decreased constriction of blood vessels.
In addition, supplementation with CoQ10 has been found to improve endothelial function in patients with type 2 diabetes mellitus. Endothelial function refers to the function of cells lining the blood vessels. CoQ10 also improves cardiovascular outcomes in patients with or without kidney disease.
Finally, a CoQ10 supplement was even found to improve serum creatinine levels, which are a marker of kidney function. As kidney disease progresses, blood creatinine levels rise.
These studies show that the answer to the question “Is CoQ10 safe for kidneys?” is a resounding yes!
What is the Best CoQ10 Dosage for Kidney Health?
Studies that looked at CoQ10 dosage established its safety and tolerability in the normal population. Doses as high as 3,000 mg per day did not produce serious side effects in normal subjects. Gastrointestinal side effects were the most common. That means CoQ10 is generally safe for healthy people, even at unusually high doses.
In kidney disease, the doses that were studied ranged from 100-300 mg daily. It is, therefore, reasonable to target a dose of 200-300 mg daily split into three doses (100 mg three times a day). Since CoQ10 is fat-soluble, it is better absorbed along with the intake of fatty foods. As always, we recommend choosing high-quality supplements.
Serum CoQ10 levels are widely available and can be measured as part of routine bloodwork. A target blood level of CoQ10 of 4.1 micromol/L was found to be therapeutic. Studies also showed that blood mononuclear cells (a diverse mixture of immune cells) may be better for monitoring its levels.
The Bottom Line on CoQ10 Dosage and CKD
CoQ10 can be beneficial for patients with kidney disease. It may improve cholesterol levels and blood pressure control and decrease oxidative stress, as well as potentially improve renal function. A dose of 200-300 mg daily divided into three doses (100 mg three times a day) is recommended for patients with kidney disease. Consult with your integrative kidney specialist to customize your CoQ10 dosage, especially if you are on medications that deplete CoQ10.
Download Your Copy!
A high intake of ultra-processed food is associated with a 24% increased risk of developing kidney disease
In this study published ahead of print, researchers studied 14,679 middle-aged adults without CKD at baseline in the Atherosclerosis Risk in Communities (ARIC) study. They divided them according to their ultra-processed food consumption into 4 quartiles.
During a median follow-up of 24 years, there were 4,859 cases of incident CKD. After adjusting for a range of confounders including lifestyle factors, demographic characteristics, and health behaviors, participants in the highest quartile of UPF consumption had a 24% higher of developing CKD compared to those in the lowest quartile.
Substituting one serving of ultra-processed foods with minimally processed foods decreased the risk of CKD by 6%.
Join us to end the kidney disease epidemic and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
Coffee consumption is associated with a decreased risk of acute kidney injury
The same cohort of the ARIC study above was evaluated for the risk of developing acute kidney injury (AKI) according to their coffee consumption (cups/day).
1694 cases of incident AKI were noted during the 24 years of follow-up. Drinking more than 2 cups of coffee a day was associated with a 17% less risk of developing AKI. This association remained significant after adjusting for all other variables.
45% of CKD patients are on potentially inappropriate medication
In a study of 375 patients published in Clinical Nephrology, patients with chronic kidney disease (CKD) were checked for potentially inappropriate medications (PIM). PIMs were checked based on kidney function (PIM-K) and age (PIM-E).
PIM-K were defined by prescription instructions of product labeling, while PIM-E were defined by BEERS, PRISCUS, and FORTA criteria. If you are not familiar with these criteria, you can learn about them here.
44.5% of all CKD patients had PIM-K. The risk for PIM-K was increased by 3.8 with 10 or more prescriptions and by 8.7 with an eGFR below 30 mL/min/1.73m2.
This study emphasizes the importance of caution and paying special attention to medication prescribing in CKD and elderly patients.
[ux_latest_products columns=”4″ title=”Download Your Copy!”Join here to receive FREE monthly updates on the latest research in Integrative Nephrology, and tips on managing kidney disease straight to your inbox.
We would love to hear your feedback. Let us know what you think of these educational materials and if you like us to focus on certain topics. Email us at info@inkidney.com
The post June Research And News appeared first on Integrative Kidney.]]>
Toxins are lurking everywhere
More than 84,000 new synthetic chemicals have been registered with the US Environmental Protection Agency (EPA) over the past 40 years. The agency tracks 775 chemicals on their “toxic release list.” These chemicals are known to cause acute or chronic human health conditions. Many of these chemicals find their way into our tap water and our produce. They are used in food processing and textile and household maintenance products. They are even present in medical and dental tools and implants.
Ten steps to decrease exposure to harmful chemicals that can cause kidney disease
So, short of living on an isolated island away from any civilization, we are all exposed to these toxins to some degree. Since these chemical exposures are inevitable, it is important to take every step possible to decrease them. These steps include:
1. Avoid using pesticides and herbicides in your home and garden: many of these contain harmful chemicals that can lead to kidney damage and decreased renal function. In this study of the National Health and Nutrition Examination Survey (NHANES) database, a commonly used pesticide was linked to chronic kidney disease. Glyphosate, which is used in a common commercially available herbicide, has been linked to CKD in Sri Lanka. To date, there are no data about it in the US.
Join us in the fight against kidney disease and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
2. Filter water with reverse osmosis (R/O) and carbon filter: Sadly, most of these chemicals have made it to our tap water. The Environmental Working Group studies water quality in various regions of the US. By plugging in your zip code here, they give you a report of the chemicals present in your city. Installing a R/O and carbon filter in your house will remove the majority of these chemicals. If installing a whole R/O unit is too expensive, try using a high-quality water filtration pitcher such as Clearlyfiltered.
Download Your Copy!
3. Use non-toxic cleaning products: Many cleaning products contain volatile chemical compounds that are especially irritating to the eyes, throat, and lungs. But many chemicals that are present in these cleaning products are also linked to kidney disease.
4. Use nontoxic building materials and carpets whenever possible: Many building materials and carpets contain toxic chemicals such as arsenic and perfluorinated compounds that have been linked to kidney disease. For a list of chemical-free building materials, check out this link.
5. Use “natural” cosmetics, nail polish, and fragrances: Investigators in Beijing looked into the manifestation of chronic mercury poisoning in 172 patients. Of these patients, 26.74% had kidney injury and three out of four were women. The most common source of exposure leading to kidney disease was cosmetics. Use the Environmental Working group (EWG) database to guide you with your cosmetics choices.
6. Consider “organic whenever possible” in food but prioritize organic meat and dairy. Many food products are contaminated by pesticides, herbicides, and other chemicals that are present in the soil. However, we understand that eating all-organic can be expensive. You can depend on the EWG, which publishes an annual list of the “Dirty DozenTM,” the shopper’s guide to pesticides in produce. You can purchase their list of the “Clean 15TM.”
Download Your Copy!
7. Be careful with consumption of large predator fish: Ciguatera is a toxin that naturally occurs in algae. Fish that eat the algae become toxic. The effect is amplified up the food chain so that the largest predatory fish are potentially the most toxic. While Ciguatera is not directly toxic to the kidneys, it can lead to severe GI symptoms that can cause dehydration and acute kidney injury. More concerning, though, is mercury in the fish. Chronic mercury poisoning can lead to nephrotic syndrome, a kidney disorder that causes the body to excrete too much protein in the urine. Limit your consumption of fish to no more than two servings a week.
8. Do not get amalgam fillings and/or consider removal: Here again, there is the potential exposure to mercury leading to kidney injury. Amalgam fillings release low levels of mercury in the form of a vapor that can be inhaled and absorbed by the lungs. According to the FDA, the highest risk population are children, pregnant and nursing mothers, patients with neurological and kidney dysfunction, and those who are sensitive to mercury. Remove mercury fillings only under the care of a dentist specifically trained in this technique and who is aware of the risks.
9. Avoid living near highways: Living near heavy traffic is associated with higher exposure to air pollution. PM 2.5 refers to particulate matter that is up to 2.5 microns in size. Because of their small size, they are considered to be the worst of all air pollutants. They reach the alveoli of the lungs and enter the bloodstream. This studylooked at the link between PM 2.5 and chronic kidney disease (CKD) in the twin cities area of Minnesota. Researchers found that the risk of CKD increases with higher levels of PM 2.5. This remained true after adjusting for all other variables.
10. Clean furnace filters regularly; consider an air purifier: Air pollution is not limited to outdoor exposure; 4.1% of global deaths are attributed to indoor air pollution. According to the EPA, fuel-burning combustion appliances, central heating, and cooling systems, and humidification devices are some of the major causes of indoor air pollution.
The bottom line on environmental chemicals and kidney disease
Environmental toxin exposure is associated with poor kidney health. There are steps that you can take to limit your exposure as much as possible. Some of these steps may not be available to you at this time or may not be easy to implement all at once. The goal is to lower the overall burden of chemicals that can cause kidney disease. It takes time. Start with one of the steps here and refer back to this guide as you gradually incorporate each of these ten steps to reach a cleaner living and healthier kidneys.
In this new category, we will post once a month practical tips and tricks for healthy living with kidney disease. Consider these as tools that you can modify according to your unique situation. These tools span across our principles of Integrative medicine approach for kidney disease, including genetics, environmental exposure, gut health, lifestyle and others. We invite others to contribute to this category. If you are interested in contributing, please contact us info@inkidney.com.
The post What Chemicals Can Cause Kidney Disease and Ten Steps To Avoid Them appeared first on Integrative Kidney.]]>

Inflammation in CKD
By Majd Isreb, MD, FACP, FASN, IFMCP
Causes of inflammation in chronic kidney disease
Inflammatory markers were found to be elevated in CKD. The levels of these markers increase with the decrease in kidney function. They also increase with increasing urine protein (albuminuria).
There are several reasons for immune imbalance and inflammation in CKD. Some of these factors are linked directly to the cause of CKD, while others are related to genetic predisposition and epigenetic factors.
Uremic environment
Furthermore, the accumulation of uremic toxins in CKD leads to oxidative stress. We discussed oxidative stress in a previous blog. When oxidative stress (or free radicals) builds up and aren’t handled properly, they can damage enzymes, cells, and tissues. Oxidative stress has been identified as a root cause of many diseases, including heart disease, Alzheimer’s, Parkinson’s, chronic kidney disease, and many more.
The build-up of harmful oxidative toxins in advanced CKD is associated with another problem which is described as “carbonyl stress.” Here, there are irreversible changes in many proteins leading to loss of their function. Higher oxidative and carbonyl stress is linked to inflammation in CKD. It is possible that carbonyl stress is just a biomarker of oxidative stress in CKD and not an independent phenomenon.
Download Your Copy!
Metabolic acidosis
Metabolic acidosis and high dietary acid load are very common in CKD. In metabolic acidosis, there is an increase in blood acidity. The foods that we eat may generate blood acidity (such as animal proteins) or alkalinity (such as fruits and vegetables). This is described as the dietary acid load We discussed these in a previous blog. They play an important role in the bone disease and protein-energy wasting that are common in CKD. In addition to that, a higher dietary acid load has been linked to faster progression of kidney disease. Metabolic acidosis has been linked to inflammation in CKD. In fact, higher inflammatory cytokines were seen in patients with metabolic acidosis.
Oral disease
Oral and periodontal disease (gum disease) are common in CKD. Over 700 species of microbes reside in the mouth. Together, they are called the oral microbiome. This microbiome produces metabolic by-products in the mouth. Some of these leaks into the bloodstream and lead to low-grade systemic inflammation.
Studies have shown that patients with severe gum disease have elevated levels of pro-inflammatory mediators and increased numbers of white blood cells known as neutrophils in the blood. This suggests that the inflammatory process in the mouth is affecting the whole body and probably injuring organs and tissues. In fact, successful treatment of gum disease was associated with improvement in inflammatory markers.
Intestinal dysbiosis
In CKD there is something called the dysbiosis cycle. We discussed this in a previous blog. Dysbiosis is a state of the intestinal microbiota where “bad” bacteria (or other organisms like yeast or parasites) outgrow the “good” bacteria. In dysbiosis, we see a rise in inflammatory markers that interact with the lining of the gut and result in damage and increased intestinal permeability (also known as “leaky gut”). “Leakiness” of the gut lining allows gut bacteria or bacterial particles from the gut into the bloodstream. It causes shifts in the breakdown of nutrients, including amino acids, which leads to the formation of many gut-derived uremic toxins. Intestinal permeability has been linked to autoimmune disease and systemic inflammation.
Vitamin D deficiency in CKD
Vitamin D deficiency in chronic kidney disease is quite common with 80% of CKD patients having been found to have low levels of 25-hydroxy vitamin D (25 (OH)D) when measured in the serum. Several factors have been implicated in the cause of this deficiency including inadequate outdoor physical activity, inadequate dietary intake, genetic variations, and loss of 25(OH)D in the urine. Vitamin D deficiency has been associated with an imbalanced immune system in CKD. This link between deficiency of vitamin D and kidney disease is important because it can lead to further inflammation in CKD.
Obesity
A higher body mass index is one of the strongest risk factors for CKD. In fact, the incidence of obesity-related kidney disease has increased 10-fold in recent years. Higher visceral fat is linked to increased protein in the urine (albuminuria). Visceral fat was also found to be associated with higher circulating inflammatory cytokines such as IL-6. This is because visceral fat cells produce these inflammatory cytokines.
Decreased clearance of cytokines
It has been well-documented that the levels of circulating inflammatory cytokines are elevated in kidney disease. Cytokines are chemical messengers that are produced by cells of the immune system. There are inflammatory cytokines and anti-inflammatory cytokines. When inflammatory cytokines are high in the blood, it is like a burning fire in the body, damaging and irritating tissues. In addition to the increased generation of cytokines in CKD, decreased renal clearance plays a significant role in the high level of cytokines in the blood.
Symptoms of inflammation in CKD
Higher levels of inflammatory markers such as IL-1beta, IL-6, TNF-alpha, C-reactive protein (CRP), and fibrinogen were found in patients with CKD, according to the Chronic Renal Insufficiency Cohort (CRIC) study. Inflammation is associated with many problems in patients with CKD. These problems include:
- Faster progression of kidney disease
- Increased protein loss in the urine
- Increased risk of heart disease and death
- Increased itching
- Worsening nutrition and protein-energy wasting
- Depression
- Worsening bone-mineral disorder
- Worsening anemia
Healing inflammation in CKD
When thinking about the best treatment for inflammation in CKD, it is crucial to address its root cause. For example, correcting the uremic environment may include strategies to decrease animal protein intake through a plant-dominant dietand a personalized gut restoration protocol. To address vitamin D deficiency, it is always recommended to check for it and correct it in all CKD patients.
Optimizing a person’s nutritional status is fundamental in healing inflammation in CKD and improving all the outcomes mentioned above. In addition, many supplements have been found to improve inflammation in CKD. These include omega-3 fatty acids, decaffeinated green tea extract, pomegranate, soy isoflavones, fiber, and probiotics.
The bottom line on inflammation and CKD
Low-grade inflammation is a common feature of CKD. Multiple root causes can be identified as a source of inflammation in kidney patients. These include decreased clearance of cytokines, oral and intestinal dysbiosis, vitamin D deficiency, uremic toxins, metabolic acidosis, and obesity. It is crucial to address the root causes of inflammation to improve kidney and heart outcomes in these patients.
The post Inflammation in CKD appeared first on Integrative Kidney.]]>By Majd Isreb, MD, FACP, FASN, IFMCP
What is oxalate?
Before we discuss the effects of oxalate on the kidneys, let’s answer the question: what is oxalate? Oxalic acid (or its ionized form, oxalate) is a simple chemical compound that humans cannot break down. It is essentially, therefore, a waste product that the body must eliminate. The kidneys are the major site of that elimination.
Despite its chemical simplicity, oxalate is actually very complex to study and understand. Most of the circulating oxalate is formed in the liver from the oxidation (the chemical combination with oxygen) of a substance called glyoxylate. Glyoxylate has two main sources. One is from carbohydrate metabolism and the other is from the degradation of collagen and protein.
While the human body cannot break down oxalate, it can use its precursor, glyoxylate, by converting it into the amino acid glycine. Vitamin B6 is a major cofactor in this conversion. This makes oxalate and glyoxylate a central link between the metabolic pathways of amino acids and carbohydrates.
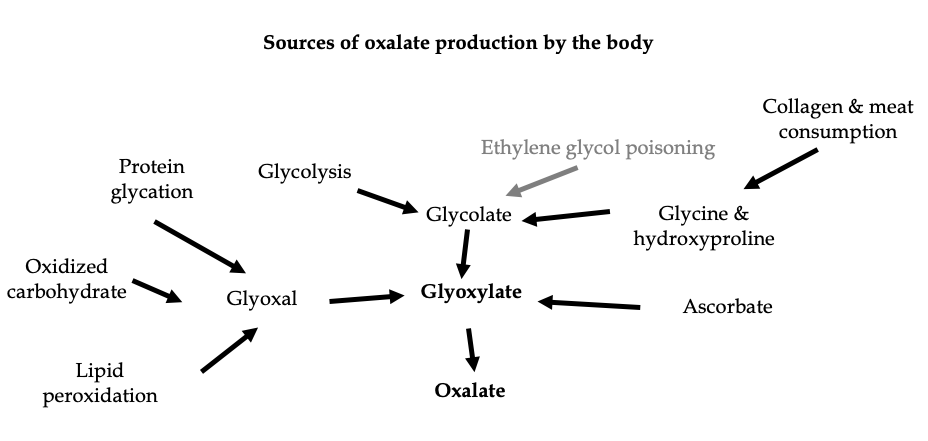
Metabolism of ascorbic acid (vitamin C) can also lead to the formation of oxalate (we will discuss this in detail in a future blog). Finally, it has been noted recently that oxalate can be generated from the breakdown of proteins, carbohydrates, or lipids that have been damaged by oxidative stress or elevated blood sugars (see figure). Oxidative stress is an imbalance between free radicals and antioxidants. The body needs some oxidative stress, but too much of it can cause problems.
All of the above pathways are responsible for 80% of oxalate produced by the body and excreted in the urine.
Download Your Copy!
Dietary oxalate sources
Dietary sources of oxalate include green leafy vegetables, different nuts, seeds, and roots, cocoa, and tea. Healthy individuals usually consume 100-200 mg of oxalate per day. The small intestine is the primary site for oxalate absorption. But it is important to realize that not all consumed oxalate ends up getting absorbed. This is because of three factors:
- Oxalate tends to bind with calcium and magnesium in the diet to form insoluble complexes that end up excreted in the stool.
- The gut microbiome contains bacteria that break down and use oxalate for energy. Probiotics containing Oxalobacter formigenes and others decreased serum oxalate levels. Diets that are high in fiber are also associated with a decrease in intestinal oxalate absorption.
- Finally, the gut can excrete oxalate.
In fact, studies have shown that in healthy individuals, only 8% of the average daily intake of oxalate is absorbed.
Elevated oxalate in the urine – hyperoxaluria
When there is excessive oxalate in the blood, the excretion of oxalate in the urine increases. This is called hyperoxaluria. Hyperoxaluria is usually defined by the excretion of more than 40-45 mg of oxalate per day in the urine.
There are two major causes of hyperoxaluria:
- Genetic (primary hyperoxaluria). Here, there are mutations in enzymes that increase the production of oxalate by the liver.
- Secondary or enteric hyperoxaluria. This occurs in patients with inflammatory bowel disorders, malabsorption, or certain bariatric surgeries. In this type of high urine oxalate, the fat that is not absorbed by the gut binds dietary calcium. This leaves soluble oxalate more available for absorption into the systemic circulation, which increases levels of oxalate.
Oxalate and Kidney disease
Oxalate effects on the kidneys
Unquestionable data shows that patients with decreased kidney function tend to have higher levels of oxalate. In fact, oxalate excretion decreases with decreasing kidney function (as measured by glomerular filtration rate, GFR).
Oxalate has been found to be inflammatory to the proximal tubules of the kidneys and it leads to interstitial fibrosis (scarring). Proximal tubules are the part of the kidney cell that recycles (reabsorbs) the molecules that the kidneys are filtering. Oxalate also binds to calcium systemically and deposits in tissues causing fibrosis in the heart and hardening of blood vessels.
What causes kidney stones?
We discussed the different types of kidney stones in a previous blog. Calcium oxalate stones are the most common types of kidney stones. Excessive oxalate in the urine can also bind calcium, forming kidney stones.
In short, excessive urinary oxalates can cause kidney stones, and oxalate and kidney stones are something that kidney disease patients need to be cautious about.
Join us in the fight against kidney disease and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
Is dietary oxalate toxic to the kidneys?
Proponents of restricting dietary oxalate tend to restrict many of the plant sources of oxalate mentioned above. It is true that there are animal models of dietary oxalate-induced kidney disease. However, these animals were fed a massive amount of oxalate and a calcium-free diet. On the other hand, it is critical to emphasize here that there are no real outcome studies that demonstrated the efficacy of a low-oxalate diet on the progression of kidney disease or even kidney stones. In fact, limiting dietary oxalate may lead to adverse outcomes such as these:
- It may be harmful to the diversity of the gut microbiome and lead to dysbiosis. The gut microbiome is the population of microorganisms that reside in the gut. An imbalance, where the bad microbes outnumber the good, is called dysbiosis. Dysbiosis can promote kidney disease.
- A low-oxalate diet limits foods that have proven benefits in kidney disease, cancer, and cardiovascular disease prevention. Every day, there are new studies confirming the benefit of a plant-based or Mediterranean diet for kidney health.
- It decreases the intake of nutritional antioxidants. Oxidative damage is a contributing factor for people with CKD.
- It reduces the quality of consumed nutrients that may contain magnesium, fiber, and alkali, which are beneficial for health.
- It does not address the root cause of kidney disease or calcium oxalate stones.
- It does not address the bigger portion of oxalate produced from animal protein and collagen by the liver, which may not be as healthy as plant-based sources.
The bottom line on oxalate and kidney disease
Oxalate levels increase with advancing kidney disease and can lead to inflammation and its faster progression. Yet, going on a low-oxalate diet is not an evidence-based recommendation for chronic kidney disease patients and could cause more harm than good. Consuming a well-balanced, whole-food, plant-dominant diet that is rich in calcium, magnesium, probiotics, and prebiotics (fibers) is more important to slow the progression of kidney disease and improve its outcomes. These dietary changes should be done under the care of an integrative team comprised of a nephrologist and dietitian/nutritionist and a coach. Join us for free to learn about the integrative medicine approach to kidney health.
The post Dietary Oxalate and Kidney Disease: Is Dietary Oxalate Toxic to the Kidneys? appeared first on Integrative Kidney.]]>
A study published in 2012 found that more than 64 million Americans aged 30 or older had periodontal (gum) disease. Gum disease, also known as periodontitis, is a severe infection of the gums caused by an immune response to imbalanced oral bacteria. Inflammation from periodontal disease can damage gums, destroy the jawbone, and lead to tooth loss. Several studies have shown an association between periodontal disease and other systemic diseases such as heart disease, diabetes, cancer, and dementia. But what about the association between dental health and kidney disease? In this blog, I am going to explore that link.

Periodontal disease and systemic inflammation
The oral microbiome produces metabolic by-products in the mouth. Some of these by-products leak into the blood stream and lead to a low-grade systemic inflammation. Studies have shown that patients with severe periodontitis have elevated levels of pro-inflammatory mediators and increased neutrophil numbers in the blood. In fact, successful treatment of gum disease was associated with improvement in inflammatory markers. Many of these inflammatory markers have been linked to heart disease, diabetes, and other diseases. This may explain the link between periodontal disease and systemic diseases.
Join us in the fight against kidney disease and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
CKD is an inflammatory state
Low-grade inflammation has been shown to be an integral aspect of chronic kidney disease (CKD). Here, too, inflammatory markers were found to be elevated. As kidney function worsens, the levels of these markers increase in the body. They also increase with increasing urine protein (albuminuria), which is common in CKD.
On the other hand, an evaluation of the Chronic Renal Insufficiency Cohort (CRIC) study found that elevated inflammatory markers were associated with rapid progression of kidney disease. So, the relationship between inflammation and kidney disease is bidirectional. CKD can lead to inflammation and inflammation can lead to and worsen CKD.
Download Your Copy!
Can gum disease cause kidney problems?
Periodontitis can increase the risk of CKD by direct and indirect effects. Directly, periodontitis increases systemic inflammatory burden leading to an increased incidence of CKD. In a recent review of 37 studies, researchers found strong evidence that periodontitis is associated with an increased risk for CKD. This association remained strong after adjusting for other risk factors.
Periodontitis can also increase the risk for CKD indirectly by increasing the risk for insulin resistance and diabetes. In this study, diabetes increased the odds of CKD by twofold, and 6.5% of this effect was mediated by periodontitis.
In addition, some of the increased risk of CKD may have to do with genetics. For example, variants in vitamin D receptor gene were associated with CKD during inflammatory conditions caused by periodontal disease.
There is not a lot of data on how treating gum disease affects CKD. However, in this pilot study, researchers found that treating severe chronic periodontitis for 180 days led to improvement of all periodontal clinical parameters. This was associated with statistically significant improvement in kidney function and markers of inflammation.
CKD and periodontitis: Does kidney disease affect oral health?
On the other hand, CKD can affect oral health by inducing gum overgrowth (known as gingival hyperplasia), dry mouth, calcification of root canals, and delayed eruption of teeth in children. These can lead to increased risk of periodontal disease. In addition, severe periodontal disease was found to be more common in patients with more severe CKD.
Kidney disease, gum disease, and nutrition
There is a triangular interaction between nutrients, CKD, and periodontal disease. Protein wasting that is common in kidney disease, for example, can increase the risk of periodontal disease. Omega-3 fatty acids, on the other hand, were found to be beneficial in the management of chronic periodontitis. Many other nutrients and micronutrients that can be altered in CKD were also associated with periodontal disease.
CKD medications may cause gum and teeth problems
Some of the medications that are used for patients with CKD can also increase the risk for periodontitis. Medications such as calcium channel blockers that are used to treat blood pressure can lead to gum swelling and overgrowth. This was also noted in some transplant medications such as cyclosporine. Other medications can be associated with dry mouth, which can promote gum and teeth problems. These include ACE inhibitors, calcium channel blockers, betablockers, and diuretics.
The bottom line on chronic kidney disease and oral health
Both periodontal disease and CKD are associated with low-level systemic inflammation. The association between the two is bidirectional. Periodontal disease can increase the risk for CKD and the rate of its progression. On the other hand, CKD can also worsen periodontal disease. Paying attention to oral health is essential for the prevention of many chronic diseases. It is also crucial for preventing or slowing down the progression of CKD.
The post Can Gum Disease Cause Kidney Problems? appeared first on Integrative Kidney.]]>Colchicine for CKD!
In a multi-center, nested, case-control study in three Korean hospitals, patients with CKD stage 3 and 4 who are using drugs including colchicine, allopurinol, and febuxostat for high uric acid or chronic gout were studied over a period of 10 years. The progression of CKD was compared between 3085 compared to 11715 control patients.
Colchicine use was associated with a lower risk of adverse kidney outcomes in CKD patients with hyperuricemia, or chronic gout.
Unlike a study published two years ago in NEJM which excluded patients with advanced CKD, this study included patients with kidney function as low as 15 ml/min. Colchicine is known to anti-inflammatory. It also protects against kidney fibrosis.
There are concerns about myopathy and neuropathy with the intake of colchicine. It is, therefore, important to adjust the dose with advanced kidney disease and to be cautious when using it with patients who are on other myopathy-inducing drugs such as statin drugs.
Join us in the fight against kidney disease and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
Long sleep duration is associated with decline in kidney function
This study is retrospective, longitudinal cohort study included 82,001 participants who visited a primary care center in Japan. Patients were categorized into CKD risk groups and sleep duration categories according to their self-reported average nightly sleep duration. The relationship between average nightly sleep duration and the incidence of composite renal outcome was studied.
Researchers found that an average sleep durations ≥8 h/night were associated with an increased risk of kidney function decline over time.
There are many reasons that connect sleep problems with poor kidney function. We summarized these in this blog.
Risk of environmental heavy metal toxicity is higher in CKD
In a study of 5,638 NHANES participants, lead and cadmium levels were higher in patients with CKD than those without it. This was also associated with decreased urinary lead excretion. Each decrease in estimated GFR by 10 ml/min/1.73m2 was associated with 0.05 mcg/dL increase in lead levels and 0.02 mcg/dL of cadmium levels. This association was even stronger among black participants.
The study concluded that CKD increases the susceptibility to heavy metal environmental exposure by reducing its elimination.
Download Your Copy!
Join here to receive FREE monthly updates on the latest research in Integrative Nephrology, and tips on managing kidney disease straight to your inbox.
We would love to hear your feedback. Let us know what you think of these educational materials and if you like us to focus on certain topics. Email us at info@inkidney.com
The post May Research And News appeared first on Integrative Kidney.]]>
Join us in the fight against kidney disease and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
Breakfast Chia Apple Oatmeal
By Majd Isreb, MD, FACP, FASN, IFMCP
This is one of my favorite breakfast recipes. It is a healthy plant-based breakfast with 7 g protein and 10 g of fiber to start you day right.

Ingredients

Direction
- Boil 1 cup of water then add oats, chia seeds and chopped apple.
- Cook for 5 minutes, stirring over medium heat.
- Sprinkle cinnamon and nutmeg.
- Add raw stevia to taste
- Add 4 oz of almond milk if desired.
- Garnish with chopped apples and blueberries (optional)
Enjoy
Download Your Copy!
The post Breakfast Chia Apple Oatmeal appeared first on Integrative Kidney.]]>








