In the wake of the current pandemic, we felt that we should share what we know about COVID-19 as it impacts kidney patients. There is a lot of misinformation out there so please be mindful of your sources. In this blog, we will focus specifically on the impact of coronavirus (COVID-19) on kidney patients and attempt to clarify best practices to prevent infection.
This is a novel virus so there is a lot we don’t know yet. We will do our best to continue to update this blog regularly as we learn new information.
What we do know for sure is that kidney disease, dialysis and transplant patients are one of the highest risk patients. So please, take it seriously. At the same time, let’s follow common sense measures to slow the spread of disease and work with public health officials to reduce hysteria.
What is COVID-19 (Coronavirus)
Coronaviruses is part of a larger family of viruses which are known to cause respiratory infections ranging from the common cold to more severe diseases such as Middle East Respiratory Syndrome (MERS) and Severe Acute Respiratory Syndrome (SARS). COVID-19 is the most recently discovered coronavirus (Coronavirus Disease 2019).
We’re still learning more about the spread of the virus, but what the research shows is that the disease is primarily spread the same way as other respiratory viruses like influenza and the common cold. The spread is from person-to-person via droplets from the nose or mouth of someone who has COVID-19 who might be coughing or sneezing. These droplets land on objects and surfaces and around another person who can breathe the virus in, or through a contaminated surface then touch their face.
The Most Common Symptoms
There are many symptoms associated with the infection and the percentage varies from report to report but here are the most common symptoms as of the last update of this blog:
- Fever, 88%.
- Dry cough, 68%.
- Fatigue 38%.
- Sputum production, 34%.
- Shortness of breath, 18.6%
Less common/rare symptoms include: Aches/pains, nasal congestion, runny nose, sore throat, diarrhea.
It’s important to be able to recognize these symptoms early to reduce risk of spreading to others. The majority of people who get infected – over 80% – will not have mild presentation and will not require medical attention or hospitalization. Also, children, while they might help spread the virus, very rarely display symptoms themselves.
What can you do?
The best course of action will always be prevention. There are a few steps you can take to protect yourself and others:
- Wash hands for at least 20 seconds, frequently. Sing happy birthday twice. Don’t forget the back of your hands, thumbs, and wrists. We cannot stress this enough since the virus can last a long time on surfaces.
- Handwashing with soap and water remains the best way to reduce germs. If for some reason they are not available, alcohol-based hand sanitizers that contain at least 60% alcohol can help to reduce the spread of infection.
- Clean surfaces thoroughly using disinfectant solution. That includes countertops, handles, cell phones and touch screens, keyboards, and remotes. Use a paper towel or elbow to open doors whenever possible.
- Don’t touch your face. This is how the virus can spread to and from surfaces.
- When you cough or sneeze, always cough into your elbow. Then wash elbow or clothing.
- Practice social distancing. Avoid crowded areas, public transportation, or social situations where you can’t maintain a distance of 6 feet (2 meters) from individuals).
- Stay away from sick people with any respiratory symptoms. COVID-19 transmission can occur via large droplet transmission (with a risk limited to ~6 feet from the patient).
Supporting your Immune System
There are some basic lifestyle and dietary practices that are more important now than ever to help support improves immune function:
- Stress reduction. Stress can reduce your immune function, making you more likely to get sick. Practice stress reduction strategies like meditation and breathing exercises to manage stress. In an attempt to educate ourselves about this outbreak, many of us are getting sucked into the news, worried about finances or loved ones. It’s very important to avoid unnecessary stress and find ways to manage our anxiety.
- Make sure you’re sleeping well. Sleep plays a big role on immune function, so it is essential to get enough sleep. Maintain consistent sleep hours, avoid the news or stressful conversations in the evening, make sure your bedroom is comfortable and cool, quiet, and dark. Consider setting a reminder to help yourself go to bed on time.
- Get consistent, moderate exercise. Regular physical activity helps to boost immune system function. Establish and follow an exercise program.
- Avoid junk food and continue to eat a nutritious diet. With more of us spending time at home to avoid contamination, the urge to snack or indulge in junk food might be higher. Continue to eat brightly colored vegetables and fruits to boost immunity and avoid highly refined, high sugar, and fired foods.
- Consider boosting immunity through supplements (talk to your doctor or pharmacist first). Having adequate levels of vitamins C, A, and D, minerals including zinc and selenium can help support improved immune response. Herbs like elderberry, garlic extract, as well as probiotics can also help boost immune function.
Although these can be helpful, they’re not specific to the treatment of COVID-19 and should not replace recommendations of your healthcare provider.
Should you see your doctor?
The healthcare system is experiencing a higher-than-usual pressure right now which makes it more challenging to have capacity to handle the expected risk in cases of COVID infection. If you are stable and have a regular follow-up appointment with your provider, it is ok to cancel and reschedule in 4-6 weeks. It’s a good idea to call your doctor to ask if there is anything they want you to do or if a virtual visit may be sufficient.
Should you stop some medications?
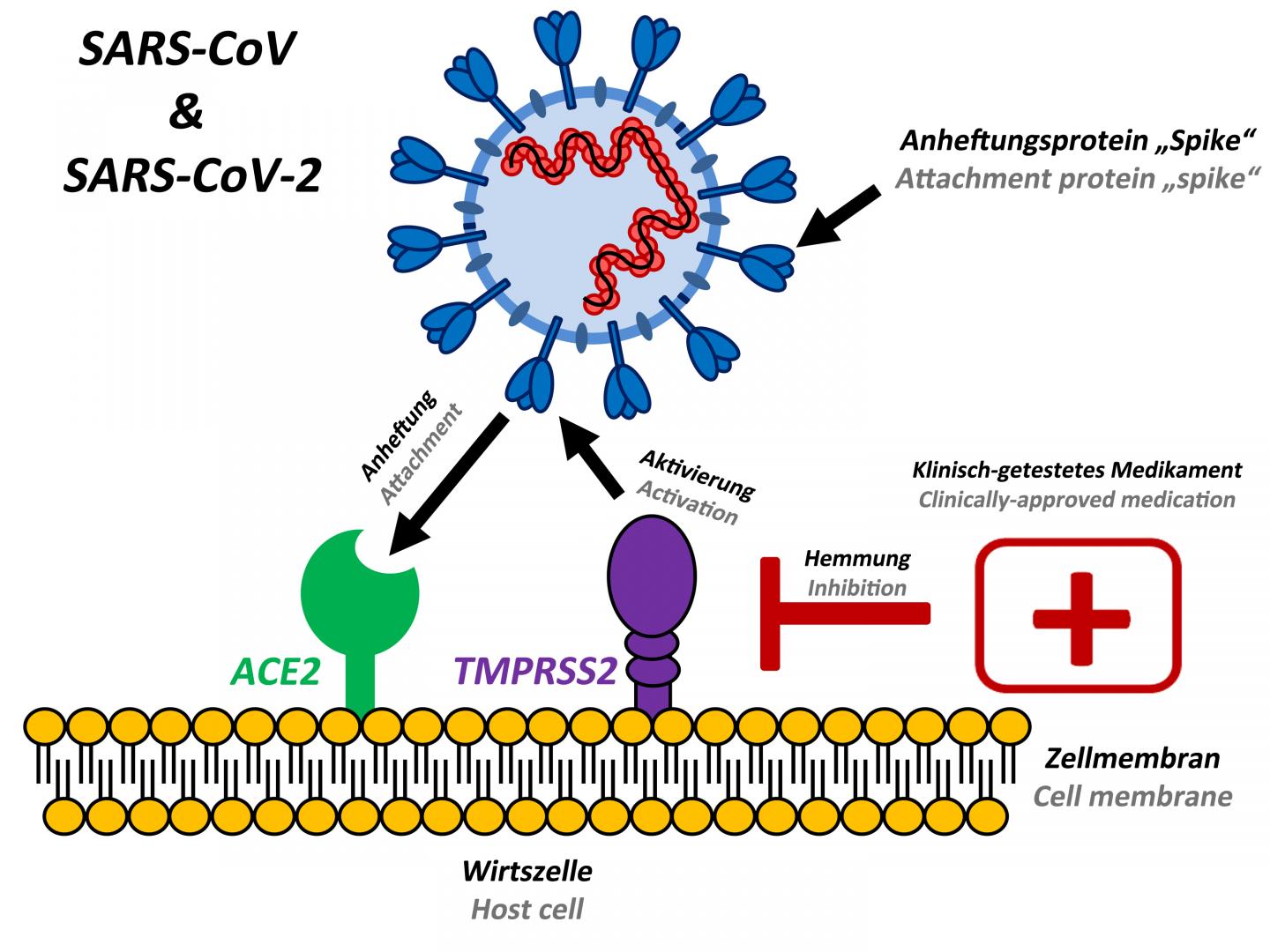
As we mention above, there is a lot we still don’t know. At this time, we know that the virus S spike binds to ACE2 receptor on lung cells. Some medications such as NSAIDs (naproxen, ibuprofen, aspirin, celecoxib, meloxicam) were found to upregulate ACE2. As you know, we already don’t recommend these medications for kidney patients for many reasons, this is another important reason to avoid NSAIDs.
There is some controversy at this time whether the class of antihypertensive medications called ACE inhibitors and ARBs can affect the risk and severity of the infection. At this time, it is believed that the risk of discontinuing these medications is too high. Do not discontinue your medication without speaking to your physician.
There is also possible genetic predisposition for an increased risk of coronavirus infection, which might be due to ACE2 SNPs that have been linked to diabetes mellitus, and high blood pressure, specifically in Asian populations. We’re still learning more on how this might impact recommendations.
What About Transplant Patients?
Kidney transplant patients (and those taking immunosuppressive agents for glomerulonephritis) should wear surgical masks when visiting a health provider’s offices. These patients are the most vulnerable and should stick to social distancing.
Some transplant centers are currently halting kidney transplant until the pandemic is controlled. Please check with your provider before discontinuing any medications.
If You Are Sick
If you start to have any symptoms, including dry cough, fever, fatigue:
- Please CALL your provider’s office before going there.
- Don’t bring your family members unless essential.
- Many provider’s offices don’t have the testing available. So, call your state COVID-19 hotline or local health department to get some guidance on local procedure.
- DON’T go to the emergency department. Hospitals and Clinics have special procedures for coronavirus, and it will help if you work with the healthcare team to follow them. Make sure you CALL before you go.
- Please don’t visit people in the hospital!
- Make sure you have a thermometer that works. Do not take ibuprofen, instead have acetaminophen, guaifenesin, and tissues on hand. Remember, the majority (over 80%) of people will only have mild symptoms they can self-treat; they don’t need hospitalization; and stay home!
What about Dialysis patients?
The recommendations for dialysis patients are similar to what we mentioned above. We must keep in mind that dialysis centers are healthcare facilities, however since dialysis patients cannot miss visits, we’ve adopted the following recommendations from Center for Medicare & Medicaid Service (CMS) recent guidelines:
- Facilities should identify patients with signs and symptoms of respiratory infections BEFORE they enter the treatment area in order to take actions to prevent contagion of virus.
- If you have a fever or respiratory symptoms, CALL ahead to the facility so they can be prepared for your arrival or triage you more appropriately as needed (for example, if they need to go to an acute care hospital).
- Patients who present with any symptoms of a respiratory infection should wear a facemask (surgical mask) at check-in and keep it on throughout their visit and until they leave the facility. The facility should provide face masks.
- Patients should inform staff of fever or respiratory symptoms immediately upon arrival at the facility at registration.
Stay healthy everyone!
This article was written with contributions from Dr. Lara Zakaria.
* The intention of this document is to educate. It is not meant to replace the recommendations of your physician of healthcare provider. Always consult your physician or healthcare provider prior to using any of these modalities. For up-to-date information on COVID-19, please consult the Centers for Disease Control and Prevention at www.cdc.gov.
The post Coronavirus and Kidney Patients appeared first on Integrative Kidney.]]>
It has been suggested that it could be due to agricultural chemicals, heavy metal exposure, silica inhalation, infectious diseases, genetic predisposition. Many of these workers regularly work in hot conditions for long hours. More recently, they identified repeated heat stress as a cause and a risk factor for kidney disease.
There is no doubt that the prevalence of kidney disease is rising in the United States (US) and throughout the world. In fact, one in seven people in the US has kidney disease. It is one of the fastest growing causes of death throughout the globe. An estimated 5–10 million people die annually from kidney disease worldwide. Unfortunately, due to poor data, lack of awareness, early detection and access to care these numbers could underestimate the exact burden of kidney disease in the world.
Chronic Kidney Disease of Unknown Origin (CKDu)
The type of chronic kidney disease that affected the agricultural workers in Central America is now called chronic kidney disease of unknown origin (or CKDu). Since the nineties, CKDu has been identified in studies of similar etiologies in Siri Lanka, India, Africa, South America and the Middle East. The common thread is the hot and humid climate.
CKDu does not follow the conventional risk factors for kidney disease and, therefore, it’s challenging to detect early and prevent. It disproportionately impacts areas with underprivileged communities and poor infrastructure. However, it would be a mistake to assume that this problem is limited to developing countries. Acute kidney injury has been reported in agricultural workers exposed to hot conditions in California and Florida.
Primary Impact: Global Temperature & Kidney Injury
It has been documented that global temperature have increased by about 1 degree centigrade (1.8 degrees Fahrenheit) in the past 50-100 years. Scientists agree that these changes have contributed with record heat waves, melting ice caps and rising sea levels, and extreme weather patterns. This pattern is posing significant health risks, some directly and some indirectly.
According to a United Nations report, climate change is expected to exacerbate health problems that already pose a major burden to vulnerable populations including children and the elderly. Climate change has been associated with a rise in many infectious diseases, especially water-borne illnesses like cholera, typhoid, and dysentery. It is also expected to contribute to the chronic disease burden and bring on new health epidemics. Not surprisingly, CKDu is one of these health issues.
Secondary Impact: Kidney Disease, Pollution, Water & Food Security
So how does rising temperature affect kidney health? The evidence points to heat stress and dehydration can result in chronic kidney disease as playing an important role in the epidemic of CKD worldwide. In fact, the progression of kidney injury has been found to worsen with rising core body temperature.
The mechanism seems to be linked with a decrease in adenosine triphosphate (ATP) levels and reduced mitochondria. These energy powerhouses are particularly abundant in the kidneys, and with reduced ATP and mitochondria, oxidative stress and cellular damage increases. Combine that with a diet with low nutrient-density and inadequate antioxidant content to neutralize oxidative stress, and risk of CKD significantly elevates. In laboratory studies, the supplementation of antioxidants prevented rats who were exposed to heat stress from developing kidney injury.
Furthermore, heat has been associated with increased risk of kidney stones and kidney stones are known risk factors for kidney disease. Since the kidneys are major site for the metabolism and elimination of toxins, exposure to toxins such as glyphosate contributes to kidney injury due to oxidative damage. Glyphosate in particular also impacts dysbiosis and gut health, which may be a confounding factor in the equation when we consider the gut-kidney connection.
As droughts become a more frequent occurrence as a consequence of climate change, dehydration from heat exposure and inadequate water consumption can lead to concentration of these toxins and, therefore, amplification of their negative effects.
Another factor to consider is the increase of pollution like heavy metal, plastics, and chemicals like pesticides and herbicides. Contamination of air and soil with pollutants increases inhalation and ingestion through food, including rise of mercury contamination in fish and arsenic in rice for example. These toxins have been associated with the rise in incidence of KDas well as other chronic diseases like diabetes and hypertension.
Last but not least, as climate change impacts food security and farming practices, access to fresh food and produce might be compromised. This may shift consumption to processed foods with less nutrient value, including less vitamins, minerals, phytonutrients, and antioxidants needed to promote healthy kidneys. Increased consumption of processed foods also leads to reduced fiber consumption, which impacts gut health and the microbiome which might be the most significant factor as we’ve discussed in our blog on the gut-kidney connection.
Other Considerations
It may sound like a cliché, but hydration is key. For those in labor industries or who work in agriculture or at increased risk of extended heat and chemical exposure, extra effort should be made to adequately hydrate. Broader public health measure and policy should be put in place to improve worker safety.
The risk increases for those taking medications that:
· Increases risk for dehydration, including diuretics (furosemide, hydrochlorothiazide, etc) or SGLT-2 inhibitors (canagliflozin, dapagliflozin, etc), or
· Decreases circulation to the kidneys, including ACE inhibitors (lisinopril, captopril, etc), angiotensin receptor antagonists (ARBS like losartan, Olmesartan, etc). However, as we mentioned earlier, heat lead to energy depletion in the kidneys and supplementing with antioxidants may further decrease the risk of kidney injury due to extreme heat.
Bottom Line
Rising global temperatures are posing increasing risk for kidney disease and contributing to a worldwide rise in chronic kidney disease. Extended exposure to heat and dehydration can lead to kidney injury and kidney stones. Improved hydration, improved nutrient-density diet, and use of antioxidants maybe be preventive. Other confounding factors cannot be ignored, including increased environmental pollution, factors that impact on gut health, and medications. Although individuals can take steps to reduce our carbon footprint, but broad public health measures must advocate for policy changes that reduce contributions to climate change and the resulting global health impacts.
The post Impact of Climate Change on Kidney Health appeared first on Integrative Kidney.]]>