By Majd Isreb, MD, FACP, FASN, IFMCP
The nervous system and kidney health
The autonomic nervous system describes the system that controls involuntary actions, such as heartbeat and the widening or narrowing of blood vessels. It has two components: the sympathetic system (fight or flight system), and the parasympathetic system (or the rest and digest system).
It has been long established that the sympathetic system innervates all segments of the kidneys including the blood vessels and tubules. Stimulating the sympathetic system (fight or flight) can affect blood flow to the kidneys and lead to sodium retention at the level of the tubules, resulting in the progression of kidney disease. The kidneys are also innervated by small branches of the parasympathetic (rest and digest) vagus nerve.
What is the vagus nerve?
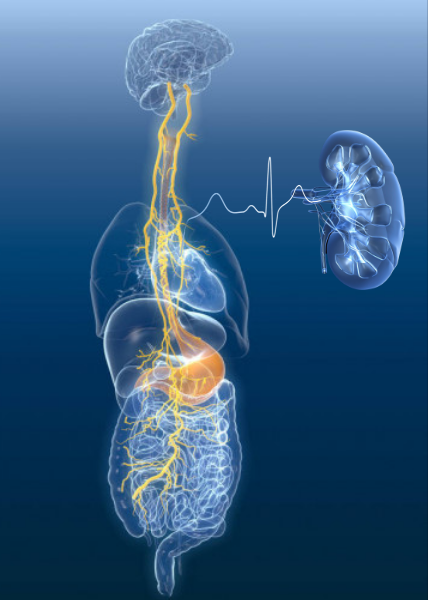
The vagus nerve is the longest nerve in the body. The word “vagus” means “wanderer” in Latin. This nerve is described as such because it connects the brain with many vital organs including the heart, lungs, gut, liver, spleen, and kidneys. It, therefore, affects breathing, digestion, and heart rate. Early studies also demonstrated that it also affects kidney blood flow.
Fascinating new evidence shows that the vagus nerve plays an important role in modulating inflammation in the body. When foreign particles are identified in various organs, “inflammatory signals” or neural messages are conveyed to the brain by the vagus nerve. The vagus nerve, then, transmits reflex signals back. These signals end up activating the splenic (spleen) nerve, which leads to a decreased inflammatory response and reduced inflammatory cytokines.
Simply put, the vagus nerve identifies triggers for inflammation and helps the brain regulate the inflammatory response. This is an evolving field called the cholinergic anti-inflammatory pathway (CAP).
Download Your Copy!
Stress worsens kidney disease
Our increasingly stressful lives can lead to increased cortisol levels, insulin resistance, and inflammation. Stress has been linked to imbalances between the sympathetic and parasympathetic systems. This is often described as autonomic dysfunction. These imbalances can also lead to the development and progression of kidney disease. Genetics, environment, and nutrition play important roles in augmenting these changes.
Autonomic dysfunction is a common finding in CKD. It is often measured by what is called heart rate variability (HRV).
Join us to end the kidney disease epidemic and receive the FREE Report “5 Pitfalls to Avoid When Caring for Kidney Patients”
Heart rate variability as a measure of vagus nerve activity
HRV is simply a measure of the variation in time between each heartbeat. Because this variation is controlled by the autonomic system, HSV can be used to measure changes in this system. The vagus nerve plays an essential role here since it controls heart rate. Therefore, stimulation of the vagus nerve can affect HRV.
HRV can be measured by analyzing a long strip of electrocardiogram (EKG). However, several companies created “apps” and heart rate monitors that can measure it. Unfortunately, the accuracy of these apps and wearable devices is not yet clear. The easiest way to check HRV is to buy a chest strap heart monitor (Polar, Wahoo) and download a free app such as Elite HRV to analyze the data. Chest straps tend to be more accurate than wrist or finger wearables.
Finally, decreased HRV has been linked to bad outcomes in hypertension, systemic inflammation, depression, and CKD. Low HRV can increase the risk of sudden cardiac death. Therefore, there is increasing interest in manipulating heart rate variability by stimulating the vagus nerve.
Activate the vagus nerve to calm inflammation in CKD
Vagus Nerve Stimulation
CKD is a state of chronic inflammation that is associated with heart disease and poor outcomes. As mentioned above, the vagus nerve plays an important role in detecting and calming inflammation in the body. It identifies sources of inflammation and helps the brain modulate the inflammatory response appropriately. The vagus nerve may play an anti-inflammatory role in conditions such as endotoxin-induced sepsis, arthritis, and acute kidney injury.
Electrical stimulation of the vagus nerve is the most common method to modulate the inflammatory response and other functions of the vagus nerve. Pharmacological methods are also being studied for that purpose. However, there are many simple and natural ways to stimulate the vagus nerve.
Natural ways to stimulate the vagus nerve
Stimulating the vagus nerve can improve the response to emotional and physiological stress, thereby improving kidney health. It can also help decrease inflammation. In fact, the FDA approved a surgically implanted device that stimulates the vagus nerve to treat resistant depression. However, there are many ways to stimulate it naturally. I will mention them briefly here.
Activate the Vagus Nerve Naturally to Improve Kidney Disease:
- Cold exposure such as cold showers.
- Deep and slow breathing can activate the parasympathetic system.
- Singing, humming, chanting, and gargling can also activate the vagus nerve because it is connected to the vocal cords.
- Probiotics, interestingly, can be beneficial in activating the gut-brain axis and stimulating the vagus nerve.
- Meditation has been found to increase vagal tone and positive emotions.
- Omega-3 fatty acids have yet another great benefit- increasing vagal activity.
- Exercise is of course linked to better mental health and stimulation of the vagus nerve.
- Massage therapy has also been found to be associated with improved vagal tone.
- Socializing and laughing can also be beneficial.
The Bottom Line
Emotional stress can be associated with faster progression of CKD. The kidneys have both sympathetic and parasympathetic innervation. Acute stress can worsen kidney function, while relaxation practices can promote kidney health. Stimulating the vagus nerve can turn on the parasympathetic nervous system, improving renal blood flow and modulating inflammation in CKD. Stress reduction and the natural stimulation of the vagus nerve can help delay the progression of kidney disease.
The post Natural Treatments to Improve Chronic Kidney Disease: Vagus Nerve Stimulation appeared first on Integrative Kidney.]]>
Only Hyperuricemia with Crystalluria, but not Asymptomatic Hyperuricemia, Drives Progression of Chronic Kidney Disease
Does elevated uric acid blood levels without symptoms of gout affect the progression of kidney disease?
A new study tried to answer this question. Previous data suggested that elevated asymptomatic uric acid could be a risk factor for the progression of CKD. However, a recent study published in NEJM last year 6/2020) found no benefit from lowering uric acid using allopurinol to slow the progression of CKD.
This new study found that it is not about the level of uric acid in the blood but about the presence of uric acid (UA) crystals in the urine. UA crystallizes in the kidney. UA crystals contribute to CKD progression because UA crystals trigger M1-like macrophage-related interstitial inflammation and fibrosis.
This study points to the limitation of conventional research that doesn’t look into the individual characteristics of each patient and point to the importance of using the simple and inexpensive urinalysis to help guide risk assessment and approach to managing uric acid in CKD.
https://jasn.asnjournals.org/content/31/12/2773
Association Between Midlife Physical Activity and Incident Kidney Disease: The Atherosclerosis Risk in Communities (ARIC) Study
Fresh from January’s American Journal of Kidney Disease:
Physical activity decreases the incidence of kidney disease… not surprisingly
Making lifestyle changes can be challenging, but are an important part of the fight against kidney disease. It can be a challenging process but understanding the brain’s efficacy and patterns can help individuals make the changes needed to lead a healthier lifestyle. Read more on our blog.
https://pubmed.ncbi.nlm.nih.gov/32971191/
Effect of Kidney Function on Relationships between Lifestyle Behaviors and Mortality or Cardiovascular Outcomes: A Pooled Cohort Analysis
In this study, investigators found that lifestyle modifications can reduce the risk of cardiovascular disease in patients with kidney function. They looked at smoking cessation, maintaining normal BMI, physical activity, healthy diet and moderate consumption of alcohol individually and in combination. Beside smoking cessation and physical activity, other individual lifestyle modifications were not sufficient alone according to this study. This emphasizes the importance of an integrative approach to kidney health and disease.
https://jasn.asnjournals.org/content/early/2021/02/04/ASN.2020040394
Laxative Use and Risk of Dyskalemia in Patients with Advanced CKD Transitioning to Dialysis
In this article, researchers found that using laxatives alone can help maintain potassium balance in patients with advanced kidney disease. The colon can actually play an important role in potassium excretion. That is one of the many reasons why a diet high in fiber is essential for kidney patients.
https://jasn.asnjournals.org/content/early/2021/02/04/ASN.2020081120
The post March Research and News appeared first on Integrative Kidney.]]>





